Telehealth Newsletter
Official Newsletter of Telemedicine Society of India

What is New?
The Odisha Chapter of TSI held its annual conference in Puri this month, and as President, I had the privilege of attending. It was inspiring to witness the energy and passion that Dr. B. N. Mohanty brings to the chapter. Under his leadership, a strong pipeline of future leaders is being nurtured-individuals who will undoubtedly carry the torch forward.
I observed a similar spirit of enthusiasm in Ahmedabad last month, particularly around digital health initiatives. These experiences reinforce the strength and potential that exists across our chapters.
As a central body, we must find ways to bring these champions together at the national level and actively engage them in our broader initiatives. This remains a challenge-one that perhaps deserves a dedicated discussion with stalwarts from different chapters. Jaipur could be an ideal setting for such a conversation.
This issue brings together a selection of articles on digital health, reflecting the growing momentum in this space. We have also included a brief report about the inauguration of West Bengal Chapter by our President Elect Dr.Murthy and from the Telangana chapter, highlighting their recent activities and contributions.
Thank You
Dr. Sunil Shroff
Chief Editor
President, TSI

Dr. Google Is Out and Dr. AI Is In: The New Patient Journey
Dr. Sunil Shroff
President, Telemedicine Society of India | Consultant Urologist & Transplant Surgeon
A recent report from West Health–Gallup (2026) study showed the rapidly changing patient behaviour when it comes to consulting technology platforms before visiting a doctor. The Gallup showed that 1 in 4 Americans—about 66 million people—now use AI tools for health advice, often before or after seeing a doctor, and sometimes instead of one.
This marks a decisive shift: patients are no longer just searching for information—they are consulting AI.
The New Patient Journey
The traditional pathway:
Symptom → Doctor
is rapidly becoming:
Symptom → (Dr.Google – previously) → Now – Dr.AI → Doctor →Dr.AI → Decision
59% use AI before a consultation
56% use it after
14% have skipped a doctor visit based on AI advice
AI is now the first touchpoint in healthcare.
What’s Changing in Patient Behaviour?
Patients today arrive:
More informed—with possible diagnoses and treatment options
More confident—46% say AI helps them engage better with doctors
More selective—weighing whether a visit is needed at all
But this confidence is not always accurate. Trust in AI remains mixed, and concerns about unsafe advice persist.
Where Does This Leave “Dr. Me”?
The doctor’s role is not diminishing—but it is transforming:
From information provider → interpreter of AI insights
From authority → collaborator with informed patients
From gatekeeper → guide ensuring safe, contextual care
In a world where answers are abundant, clinical judgment and trust become the true differentiators.
What About Hospital Visits?
AI is quietly reshaping healthcare utilization:
Potential reduction in minor, low-acuity visits
More complex consultations with pre-informed patients
Risk of delayed care when AI replaces timely medical advice
The “front door” of healthcare is no longer the clinic—it is increasingly digital and AI-driven.
The Takeaway
The rise of Dr. AI is not a threat—it is a signal.
A signal that:
Patients want faster, accessible, and understandable care
Healthcare systems must adapt to a new first point of contact
Doctors must evolve from being the first source of information to the most trusted source of truth
Final Word
The future is not Doctor vs AI.
It is:
Doctor + AI + Patient
And in that equation, the success of Dr. Me will depend on one thing:
Staying the most trusted voice in an AI-first world.
(This article is summary of the article – After Dr. Google, It Is Dr. AI — Where Does It Leave Dr. Me? from www.medindia.net by the same author)

Digital Health Conferences: Trials & Tribulations
Dr. K. Ganapathy
Hon Distinguished Professor IIM Jammu
Distinguished Professor, The Tamilnadu Dr MGR Medical University
Emeritus Professor, National Academy of Medical Sciences
Formerly Distinguished Visiting Professor IIT Kanpur
Past President, Telemedicine Society & Neurological Society of India
Formerly WHO Digital Health expert
“In our rush to build shovels, we should know what we are digging for”
I started attending neurosurgical conferences from 1975. Over the last 28 years, was actively involved in organising conferences and for many years was the Principal Organising Secretary – but that was for neurosurgical conferences in the BC era. In the last 15 years have also helped draw up the scientific program for a major International Digital Health conference. Though a staunch advocate of “TELE”, even in the virtual AI enabled universe, physically listening to experienced speakers, visiting trade exhibitions and just meeting like-minded friends and colleagues, goes a long way in augmenting every one’s personal growth and development.
Nevertheless, can a hard-core clinician of yesteryears, advise future ready, gizmo making healthineers, particularly when the RoI expected in speaking and attending Digital Health conferences, is quite different. Excellence is a moving target. The bar needs to be raised every year. Attendees increase, if quality and quantity of presentations increase, in breadth and depth, for the beginner and for the expert. Starters, main course, dessert, a focused menu offering an intellectual repast – 20 hours of unadulterated wisdom – easier said than done! One must accept that in the real world “All are equal, but some are more equal”
Today, in any conference dealing with any aspect of healthcare, AI must be used, as a suffix and prefix. Hyperboles and embellishments are necessary marketing tools. Doctors are told to lead the AI transformation, before patients start demanding and even using it! Challenges in organising a Digital Health conference cluster around governance, scientific program design, logistics and stakeholder management. Balancing “digital health for clinicians” vs health-IT, start-ups, MedTech, policy and investors in one single event, risks a fuzzy value proposition. Tracks and audiences need to be clearly segmented. This requires a strong local organising committee, scientific committee and exhibition/trade committee. While implicit trust in a professional conference organiser is essential there must be a fine balance between delegation and micromanagement.
Raising adequate funds in time is a gargantuan task. Late sponsorship confirmations and slower registrations can produce cash-flow stress. Managing industry sponsorship in line with ethics can constrain how sponsors are acknowledged and given prime stage time. Differentiating between “whose bread you eat, his song you must sing” and a globally renowned domain expert an academician par excellence, is not simple. Having parallel sessions presupposes having adequate capacity multiple halls. How does one ensure equitable audience distribution. No speaker wants to be the first speaker or last speaker or immediately after lunch. The organising secretary must factor in distance from the airport, traffic jams, unexpected bandhs and of course snowstorms in different parts of the world. It is expected that the chief of staff of global MNC CEO’s have ensured that their bosses have valid visas. It is amazing how the PMO holds emergency meetings at exactly the time when a Secretary to the Govt of India has agreed for a keynote address. Every session should have a specific theme and all talks covering a theme should be in that session. However, it is astonishing that some speakers in that session have flights to catch at that time . Having a pot pourri of unrelated topics in one session, to accommodate such speakers, raises eyebrows! With 65 speakers, not sure if Perplexity or ChatGPT 5.1 could give correct weightage to the scores of unpredictable variables and produce a conference to satisfy most of the attendees and speakers from a diversified background, with different expectations !
To add to the complexities, VVIP’s only confirm their participation hours before they are expected, even though the invitation was extended a year earlier. As they do not decline, alternative arrangements cannot be made. No VVIP likes to be in the 12th Man / RAC category . Hence there can be no back up plan! Murphy’s law ( if a thing can go wrong it usually will ) is particularly applicable to airport transfers and hotel checking. Delegates do not reply to multiple reminders of early check in and late check out requirements and fume and fret for the 300 seconds waiting time.
Wi-Fi, app based programmes, QR check-in, CME credits , catering to wide culinary tastes covering gluten and peanut allergy and special needs are in 2026, the basic expectations. Exhibitors expect footfall, speaking slots, lead capture support, and visible branding. Registration management should include spell checks, accurate attendee lists, handling payments, GST invoices and on-site badge printing. Recruiting and training enough volunteers for hall management, speaker support, and delegate help desks is essential. Despite all this a passionate dedicated group of NI enabled humans can still do wonders and organise successful Digital Health conferences .
Report of 14th Annual Conference of The Telemedicine Society of India (TSI), Odisha Chapter (Oditelemedicon 2026) held on 18.04.2026 at Puri, Odisha.
Dr.Biswajit Samal
Hony.Secretary, TSI Odisha Chapter
The 14th annual conference of The Telemedicine Society of India (TSI), Odisha Chapter (Oditelemedicon 2026) was organized by TSI, Odisha Chapter in association with District Health Administration, Puri as a hybrid event on 18th April 2026. The venue for the conference was District Training Unit-II, Dist.Hqrs.Hospital, Puri. The theme of the conference was “Telemedicine powered by modern digital technologies poised to revolutionize healthcare delivery”. A total number of 112 participants from various districts of Odisha physically attended the conference. 11 TSI members attended the conference over virtual platform.
The conference was inaugurated by Dr.Sunil Shroff, President of Telemedicine Society of India. Dr. Akshay Kumar Satpathy, CDM&PHO, Puri attended the inaugural function as guest of honour. Dr. B Nageswar Rao Subudhi, president of TSI, Odisha Chapter presided over the function. Annual Report of the chapter was presented by Odisha Chapter secretary Dr. Biswajit Samal.Chief coordinator of the conference Dr.Biswa N Mohanty delivered welcome address.
The 1st session was held on ‘Digital Solutions to meet healthcare needs’. The speakers in this session were Rashmita Samal,Senior Programs Manager, Intelehealth, Bhubaneswar; Dr.Sunil Shroff,President of Telemedicine Society of India and Mr.Sameer Sawarkar, Co-Founder and CEO, Neurosynaptic Communications Pvt. Ltd. Bangalore. Rashmita Samal delivered a talk on ‘The eSanjeevani Ayushman Arogya Mandir Platform in Odisha with support from Intelehealth- an enabler of universal access to quality healthcare services’. Dr.Shroff talked on ‘AI Innovation versus Data Protection: finding the balance in healthcare’.Sameer Sawarkar spoke on ‘Expanding access to primary care in rural and underserved areas of Odisha through its ReMeDi® technology’.
The 2nd session was held on ‘Innovations and changing clinical practice’. The speakers in this session were Dr. R Kim, Chief Medical Officer & Senior Consultant, Vitreo-Retinal Services,Aravind Eye Hospital & Postgraduate Institute of Ophthalmology, Madurai;Dr.Bidyut Kumar Das,Professor of Clinical Immunology & Rheumatology, SCB Medical College, Cuttack;Dr.Rakesh Kumar Routray, Assistant Professor of Nephrology, SCB Medical College, Cuttack and Dr.Sabyasachi Pattanaik, senior Ophthalmology specialist,Bhubaneswar.Dr.Kim delivered a talk on “Changing dimensions in the practice of Tele-Ophthalmology in India”, Dr.B K Das talked on “Impact of Rheumatology tele-care on rural population in Odisha”,Dr.Routray spoke on “Reaching the unreached : Telenephrology in Rural and Remote care” and Dr.Pattanaik talked on “Telemedicine enabled vision center for universal eye care”.
A panel discussion was held on the theme “Changing face of telemedicine and digital health for effective delivery of patient-centric care” at 2.15pm moderated by Dr.Biswa N Mohanty, Dr.Srikanta Patnaik and Mr.Sujan Kumar Mohanty. The speakers were Dr. Arun Kumar Choudhury,former professor & head, Burns and Plastic Surgery Department, SCB Medical College, Cuttack; Dr.Rajamenakshi R, scientist-F,HPC-Medical & BioInformatics applications Group from CDAC,Pune; Dr.Vivek Tiwari, Assistant Professor, Department of Biological Sciences,IISER,Berhampur and Mr.Ashwin Desai,Managing Director, A & T Video Networks Pvt. Ltd, Madurai. Dr.Choudhury addressed the issue of ‘combining in-person care and virtual care for delivery of appropriate health care’; Dr.Rajamenakshi R, Pune addressed the issue of ‘addressable cybersecurity threats for secure data sharing’;Dr.Vivek Tiwari of Berhampur discussed on ‘Generative AI for clinical augmentation’ and Mr.Ashwin Desai from Madurai addressed the issue of ‘New initiatives in patient-centric telecare’.
The chair persons for different sessions were Dr.Ramnath Misra,past-president of TSI Odisha Chapter from Bhubaneswar, Dr. I B Kar, past-president, TSI Odisha Chapter from Cuttack; Dr.B Nageswar Rao Subudhi,president of odisha chapter from Berhampur, Dr.Bijay Kumar Mohapatra past-president of TSI Odisha Chapter from Bhubaneswar and Dr.Manoranjan Patnaik past-president of TSI Odisha Chapter from Cuttack.
In-charge medical officers from CHCs and Community Health Officers from various Govt. health institutions of Puri District; IMA members of Puri branch; Teachers of SJ Medical College & Hospital Puri; Medical Officers of Puri Dist.Hqrs. Hospital, TSI members and health administrators working under Odisha Govt., telemedicine technical personnel from several telemedicine nodes of Odisha attended the conference. Some members of TSI including past-presidents, current executive committee members and other invited guests participated in the program over virtual platform from different locations.
The Annual General Body Meeting of the TSI, Odisha Chapter was held at the same venue at 1.00pm on 18.04.2026. The following life members of TSI were elected as office bearers of the Odisha state chapter for the term 2026-27.
President: Dr. Arun Kumar Mohanty, Cuttack
Immediate Past-President: Dr. B Nageswar Rao Subudhi, Berhampur
President-elect: Dr. Arun Kumar Choudhury, Cuttack
Vice-President: Dr. Sabyasachi Patnaik, Rourkela
Secretary: Dr. Biswajit Samal , Angul
Jt. Secretary: Dr.Pranab Sankar Dash, Baripada
Treasurer: Dr. Sarat Kumar Nayak, Cuttack
Executive Members : Dr. Bidyut Kumar Das,Cuttack & Dr. Sribatsa Kumar Mohapatra, Burla
The valedictory function was held at 3.30pm. Newly elected president Dr. Arun Kumar Mohanty was installed during the valedictory function. After installation the incoming president spoke about his plan of action for the coming year. The District Health Administration of Puri District represented by CDM & PHO, Puri was felicitated by President of TSI, Odisha chapter. Coordinator of the conference Dr. Sibananda Mohanty thanked profusely the district health administration of Puri for its overwhelming support to organize the conference. He also thanked all the invited speakers. In the valedictory function, participants from CHCs and sub-centers highly appreciated the TSI, Odisha Chapter for the useful discussions held during the conference which helped them immensely in enhancing their understanding of digital health applications.




Strategic Roadmap for AI-Enabled Telemedicine: A Report on the Milestone Event of TSI West Bengal Chapter Inauguration
Dr. Murthy Remilla
President-Elect, Telemedicine Society of India
(with iputs from honorable members of WB and Rappeuterts of Groups)
On March 21, 2026, I had the privilege of witnessing a landmark event in the evolution of digital health in India: the formal inauguration of the 21st State Chapter of the Telemedicine Society of India (TSI) in West Bengal. The day was characterized by a spirit of innovation, most notably through the implementation of a structured program designed to move from ceremonial opening to immediate clinical and policy action with active involvement of memebrs and prospective-members of particpants in the function.
Program Plan and Structure
The event was meticulously organized to facilitate high-level networking, formalize leadership, and engage experts in intensive problem-solving.
I. Commencement and Formalities
- Registration and Networking: Led by Hony Secretary Subir Ghosh and Executive Member Madhurima Roy, the session provided 49 delegates with essential seminar materials, including agendas, notepads, and pens.

- Traditional Welcome: Reflecting regional culture, the Chief Guest and participants were welcomed with traditional Khadas from the hills by the President, Dr. Pankaj Chowdhary.
- Inaugural Addresses and Welcome Speech: Prof. Supten, President-Elect of the TSI WB Chapter, facilitated the reception of national leadership and special invitees.
- Introduction: Subir Ghosh formally introduced the Chief Guest and diverse group of guests and participants to the house.
- Official Launch: Dr. Pankaj Chowdhary, President of the TSI WB Chapter, and Dr. Murthy Remilla, President-Elect, Telemedicine Society of India performed the traditional inauguration and declared the chapter open to takeup the objectives for TSI in Eastern India.
- Adress By Chief Guest: Dr. Murthy Remilla President-elect, TSI coveyed the message of greetings from President & EC of TSI to new chapter of WB and conevyed best wishes of the entire community of TSI members all across India in wleocming the newly formed West Bengal Chapter onbaord. Dr. Murthy briefed aboy the initiation if TM services in India with support of ISRO and the evolution and growth of TM in india including the formal formation of TSI and theregistarion. He also explained the efforts towards the issue of Telemedicine practivce Guidelines (TMPG) and the efforts by all stakeholders of TSI, setting the background and tone for the group discussions on opportunities and challenges to embrace the AI technology into Telemedicine.

II. The Round Table Framework
The structural centerpiece was the Round Table Discussions, an innovative format introduced by Dr. Pankaj and Dr. Supten probbaly first time in the histrory of any state chapter inaguration of TSI state chapter.
Discussions were arrnaged into 4 groups on 4 themes- Introduced by Dr Pankaj. Participants were divided into four specialized groups, each assigned a moderator and a rapporteur to guide 30 minutes of intensive discussion followed by a 3-minute presentation of conclusions.
Detailed Group Outcomes and Resolutions
Group 1: AI-Enabled Telemedicine for Bridging Healthcare Access Gaps
- Moderator: Dr. Saptarshi Ghosh (Med. Supt., KPC Medical College)
- Rapporteur: Dr. Sudeshna
- Core Discussion: The group addressed how healthcare inequity in North Bengal and the Northeast is exacerbated by terrain, infrastructure, and specialist shortages.
- Key Outcomes:
Intelligent Triage: Proposed AI systems capable of early symptom assessment and prioritizing cases to optimize medical resources.
Public Health Integration: Recommended embedding AI within national programs like Tuberculosis control (AI screening), Maternal Health (Tele-ANC), and NCD monitoring.
Digital Inclusion: Utilizing the Bangla Sahayata Kendra network to help citizens navigate digital platforms, with a focus on multilingual and voice-enabled AI.
Institutional Hubs: Using tertiary institutions like IPGMER and SSKM Hospital as hubs to provide specialist consultations to peripheral enters.
Group 2: AI in Continuum of Care – Chronic Disease, Oncology & Palliative Care

- Moderator: Dr. Padmawati
- Rapporteur: Dr. Pankaj
- Core Discussion: This group focused on the short-term reality of long-term care, identifying a critical need for home-based support.
- Key Outcomes:
- Immediate Pilot Project: Resolved to launch a pilot program within 2–6 months focusing on the chronic disease continuum, specifically palliative care at home.
- District Implementation: The pilot will run in one or two selected districts to evaluate real-world barriers.
- Phased Scaling: A subsequent 6–12 month plan will address discovered shortcomings through new procedures and training programs.
Group 3: Ethics, Data Governance, and Trust in AI-Driven Telemedicine

- Moderator: Dr. T. N. Sharma
- Rapporteur: Dr. Supten Sarbadhikari
- Core Discussion: Focused on the “Trust” factor, emphasizing that AI must be auditable, fair, and human-centric.
Key Outcomes (0–6 Month Roadmap):
- Months 1-2: Establish a Digital Ethics Committee and define clear Data Stewardship roles.
- Months 2-4: Implement “Privacy by Design,” data minimization, and consent management.
- Months 4-6: Ensure regulatory alignment with DPDPA, HIPAA, and GDPR.
- “Human-in-the-Loop”: Mandatory clinical validation and algorithmic audits.
- Policy Deliverable: A formal “AI in Telehealth” Ethical Use Policy for State Government approval.
Group 4: Capacity Building and Future Workforce

- Moderator: Dr. Biswajit Roy Chowdhury (SAIARD)
- Rapporteur: Dr. Ritesh
- Core Discussion: Identified the human and technical infrastructure needed to sustain a technology-ready workforce.
Key Outcomes:
- Academic Integration: Recommended introducing Telemedicine courses into the High School (HS) level curriculum.
- Clinician Adaptation: Encouraging senior doctors to adopt and adapt to new technologies.
- Infrastructural Reform: Improving satellite communication for far-flung areas and linking Aadhar with UhlD Cards.
- Policy Advocacy: Removing barriers between Central and State implementations and making the medico-legal system more flexible.
Executive Summary of Resolutions
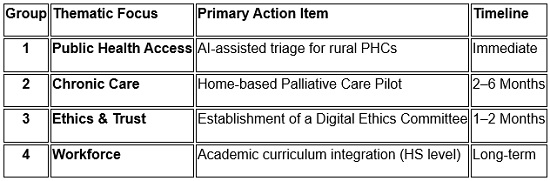
Presentation of Mementos & Certification of appreciation by the Chief Guest:

The day concluded with an open floor interaction led by Dr. Kamal Roy and Dr. T.N. Sharma, followed by the presentation of resolutions by Dr. Sudeshna and Dr. Padmawati. We have now officially formed the TSI West Bengal Telemedicine Working Group to turn these discussions into reality. Dr. Murthy Remilla President-Elect, Telemedicine Society of India requetsed non-memebrs of the participants to become Life Members/Student Members of TSI and again appreciated the members who have worked towards the formation of the state chapter. The function conculded with a formal vote of thanks and a group photo.

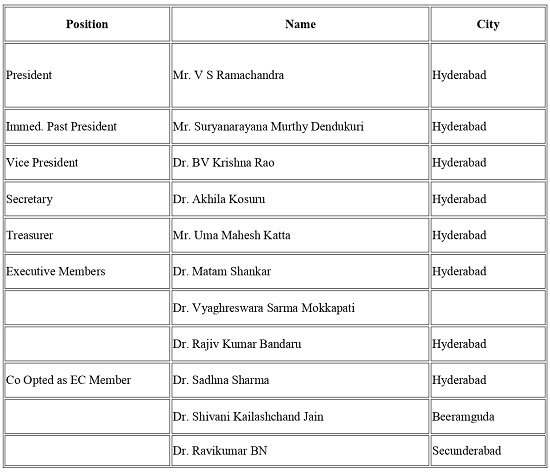
News from TSI Telangana
Dr. Krishna Rao
Wednesday, the 8th April 2026.
Maheshwara Medical College and Hospital, in association with the Telemedicine Society of India, Telangana Chapter, has initiated the Knowledge Series 2026 to bring global experts onto a common platform to share their personal and professional journeys, along with insights into technological transformations in the healthcare industry. The series not only promotes knowledge sharing but also exposes medical students to diverse platforms and verticals, encouraging them to look beyond conventional boundaries and ensuring that their education extends beyond domain-specific expertise.

As part of this initiative, the institution invited Shri Day Veerlapati, a US-based NRI, who inspired students with the spirit of innovation and entrepreneurship. He spoke about the impact of telemedicine in connecting rural communities, highlighted challenges related to international travel especially to the United States and emphasised the importance of the Triple E’s: Education, Entrepreneurship, and Enlightenment. He also encouraged meditation, self-inquiry through the question “Who am I?”, and a proactive approach towards startups. Shri Dev is an IIT Kharagpur alumnus and Founder of S2 Tech, he further stressed the value of joining platforms like Toastmasters to enhance communication skills and cultivate an entrepreneurial mindset.
The session was moderated by Shri D. Chakrapani, Retired IAS officer and Academic Advisor to Maheshwara, whose practical insights greatly enriched the discussions. The Knowledge Series 2026 has been widely appreciated for nurturing critical thinking and shaping future ready medical professionals. Maheshwara Medical College and Hospital continues to lead in integrating education with innovation, setting benchmarks in telemedicine driven learning and emerging as a dynamic platform in today’s evolving healthcare landscape.
15th April 2026, Wednesday

As part of the Knowledge Series initiative, organized in collaboration between Telemedicine Society of India (TSI) and Maheshwara Medical College and Hospital, an insightful academic session was conducted for medical students and faculty, focusing on critical and often overlooked aspects of women’s health and social wellbeing.
The session was led by Dr. Samavedam Venkata Kameswari, a senior gynaecologist and research scientist, along with Dr. Prakash Vinjamuri, who together addressed a wide spectrum of issues including women’s health in rural settings, the growing concern of unwarranted escalation of surgical interventions, and the socio-cultural challenges faced by women in villages.
Dr. Kameswari passionately emphasized her visionary campaign, “Save Uterus – Our First Home,” highlighting the urgent need to prevent unnecessary hysterectomies through awareness, ethical medical practices, and early interventions. She also underscored the importance of emotional and social support for women within families, reinforcing her powerful message: “If the woman at home is healthy and happy, the entire family thrives.”
The session was highly interactive and deeply impactful. Students and faculty actively engaged with the speakers, raising thoughtful questions and showing keen interest in the subject. Inspired by the vision and commitment of Dr. Kameswari, the students expressed their willingness to contribute to the campaign and have joined hands to promote the message of “Save Uterus – Our First Home” across villages in Medak.
This initiative marks a meaningful step toward integrating academic learning with community service, empowering future medical professionals to advocate for ethical healthcare practices and the holistic wellbeing of women in society.
17th April 2026, Friday
A Mega Medical Camp at Bonthapally village in Jinnaram Mandal of Sangareddy district, Hyderabad

A two-day mega medical camp was successfully conducted at Bonthapally village in Jinnaram Mandal of Sangareddy district on April 17th, 2026, bringing together technology-driven healthcare and community outreach. The initiative was organized under the Telangana Chapter of the Telemedicine Society of India (TSI) as part of its healthcare services aimed at extending telemedicine services and also improving access to quality healthcare in rural areas. The camp was a collaborative effort between Rejuvin Medicare technical partner, Maheshwara Medical College & Hospital – medical services partner, and Gidde Raju Charitable Trust, which provided logistical support.
The camp stood out for its use of advanced diagnostic technology, enabling patients to receive real-time, color-coded medical reports for better understanding of their health conditions. This innovation helped bring clarity to several cases, particularly in differentiating gastric issues from cardiac complaints, thereby reducing unnecessary anxiety and interventions. A team of doctors, nurses, and paramedical staff from Maheshwara Medical College provided comprehensive services including cardiology screening, diabetes testing, ENT and eye check-ups, orthopaedic evaluations, gynaecological consultations, and general health assessments through Rijuven Clinic in a Bag portable investigative kit. Free medicines were also distributed to patients in need by Maheshwara.
The initiative received an overwhelming response from the local community, who appreciated the camp not merely as a one-time medical service but as an awareness-driven approach to preventive healthcare and rational use of medicines. Encouraged by its impact, village representatives and Panchayat members have expressed interest in establishing a long-term collaboration through a formal MoU to transform Bonthapally into a model village for digital healthcare. The organizers have responded positively, signaling the potential for sustained telemedicine-driven healthcare services in the region.
When Patient Data Disappear: Ghana’s Warning to Global Healthcare Systems
A recent correspondence in The Lancet Digital Health highlights a major digital health crisis in Ghana, where clinicians abruptly lost access to electronic patient records after a contractual dispute with a foreign technology vendor. The shutdown disrupted care, delayed treatments, and compromised clinical decision-making.
The authors warn that this incident underscores a global vulnerability in healthcare digitization: when patient data are controlled by external commercial providers—especially when stored outside national borders—health systems risk losing access due to contractual, corporate, or geopolitical conflicts.
Ghana has since migrated to a national system, but the damage persists, with clinicians forced to re-enter incomplete records and manage patient safety risks. The report calls on policymakers and healthcare leaders worldwide to treat patient data as critical infrastructure, ensure sovereign control over health records, and strengthen safeguards around digital health governance.
Key Takeaway:
Patient data are not merely digital files—they are lifelines. Healthcare systems must ensure secure, sovereign, and uninterrupted access to electronic health records.
::ANNOUNCEMENTS::

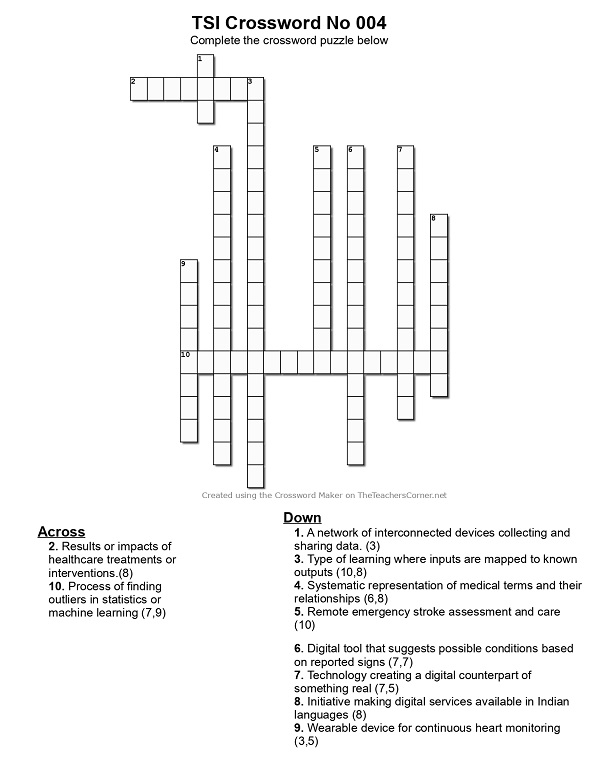
::CROSSWORD::

Click here to Print the Crossword
Click here to view the Crossword Rules and Regulations
Compiled by Dr.Umashankar
Answers in May 2026 Newsletter!
Telemedicine – News from India & Abroad
Can AI Improve Early Detection of Skin Cancer?
Can artificial intelligence (AI) spot skin cancer risk in routine health records? Yes, AI can use routinely collected healthcare data…………….. Read More
Are AI Chatbots Safe for Medical Advice?
Can we trust chatbots for medical advice when half their evidence-based answers are “somewhat” or “highly” problematic?………………… Read More
Telemedicine Practice Guidelines – A Foundation Course for RMPs by TSI Faculty
To know more about the Telemedicine Foundation Course click on the link below:
https://tsitn.org/tpg-course/
Medical Writing Certificate Course with Internship Opportunity!
TSI invites all the TSI Chapters and Members to submit information on their upcoming Webinar or Events (50 words), News related to Telemedicine (200 words) or short articles (500 words) for the monthly e-newsletter.Guidelines for submission to TSI Newsletter-
- Report can be from 500 to 600 words
- Report Should be relevant to Telemedicine or Medical Informatics
- No promotion of self or any product
- Avoid plagiarism
- All references should be included
- Provide any attributions
- Visuals are welcome including video links
- Send full authors name, degrees, affiliations along with a passport sized photograph of good resolution. If multiple authors only main author photo to be sent.
Submission may be sent to – tsigrouptn@gmail.com
Editors reserve the rights for accepting and publishing any submitted material.
Editor in Chief – Dr. Sunil Shroff
Editors – Dr. Senthil Tamilarasan & Dr. Sheila John
Technical Partner- https://www.medindia.net