Telehealth Newsletter
Official Newsletter of Telemedicine Society of India

What is New?
The National Institute of Mental Health and Neurosciences (NIMHANS), Bengaluru, has released the Guidelines on Digital Mental Health Applications following a national consultative meeting involving experts, policymakers, WHO India, UNICEF, and technology stakeholders. The guidelines provide recommendations for app developers, mental health professionals, and users to ensure safe, ethical, and evidence-informed use of digital mental health tools in India. Key focus areas include transparency, data privacy, AI disclosure, crisis support integration, professional oversight, and safeguards against emotional dependency on AI chatbots. The document marks an important step toward responsible digital mental healthcare in the country.
Last month also marked an important milestone in digital health education, as the first batch of the Certificate Course in Digital Health from The Tamil Nadu Dr. M.G.R. Medical University successfully completed the programme. Certificates were distributed during the OTICIA event, recognising the efforts of participants who completed the course and strengthened their understanding of emerging digital health technologies and practices.
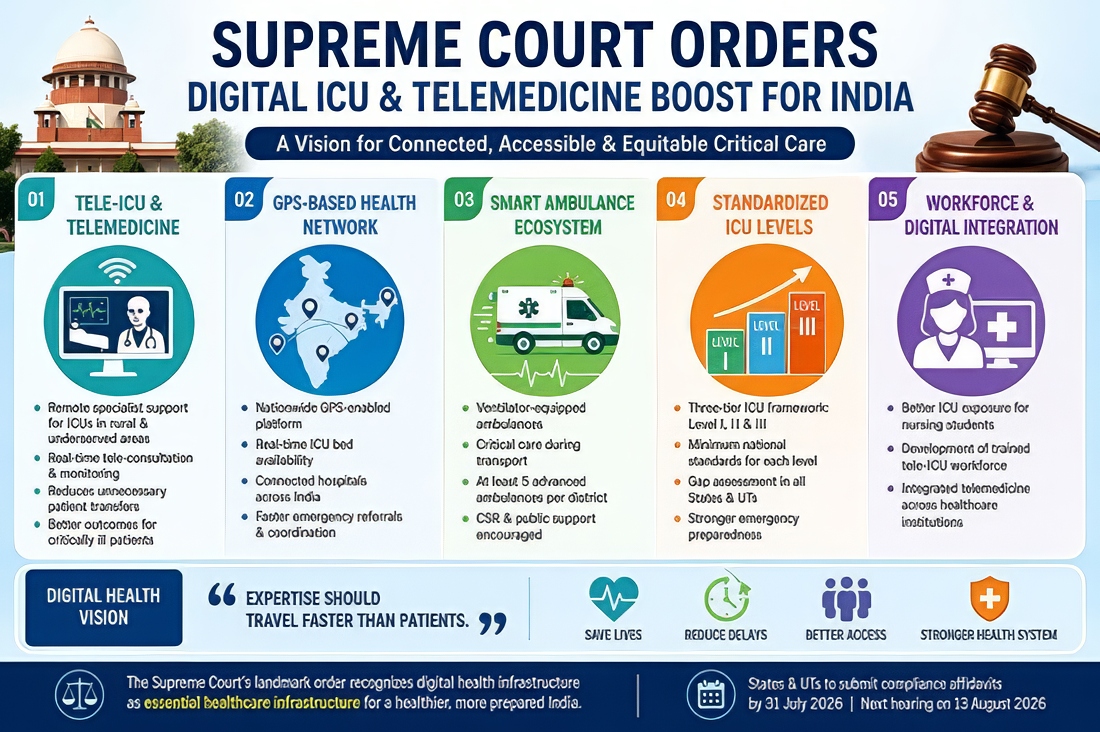
Another major healthcare development this month has been the Supreme Court of India’s landmark directions to strengthen Intensive Care Unit (ICU) infrastructure and emergency medical preparedness across the country. In its order, the Court emphasised that access to emergency and critical care is an integral part of the Right to Life under Article 21 of the Constitution. The Court approved a three-tier ICU classification system and directed States and Union Territories to conduct gap assessments of ICU infrastructure, manpower, and emergency services. It also highlighted the need for advanced ambulance networks, tele-ICU systems, GPS-enabled hospital coordination platforms, and stronger nursing training standards linked to ICU exposure. The judgment is expected to play a transformative role in improving critical care services, emergency preparedness, and equitable access to life-saving healthcare across India.
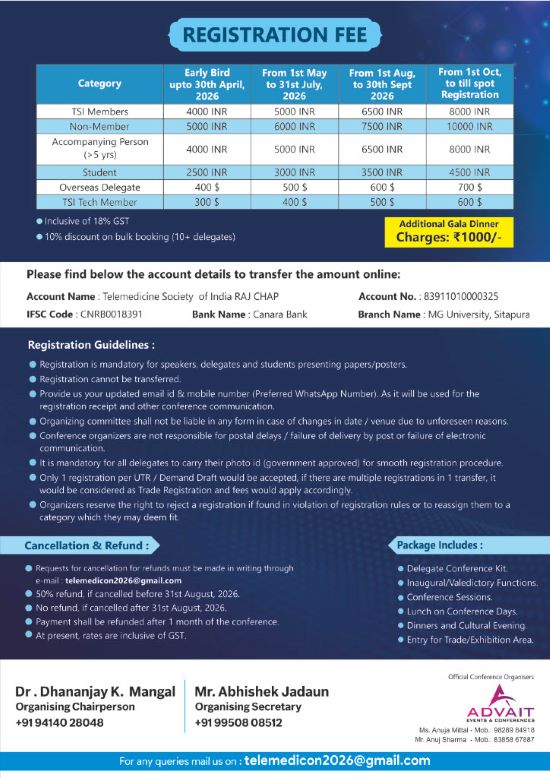
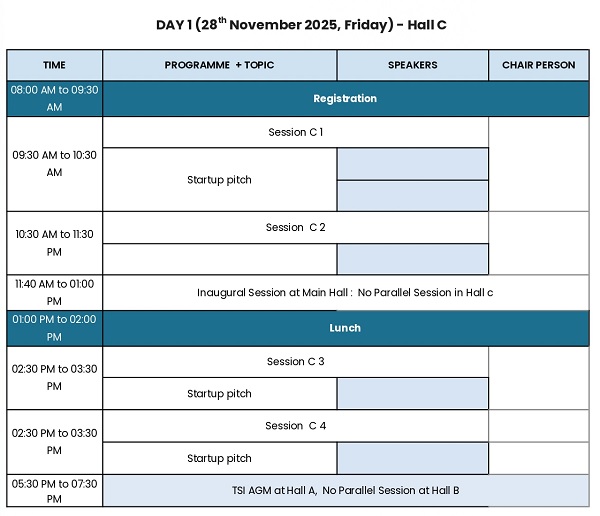
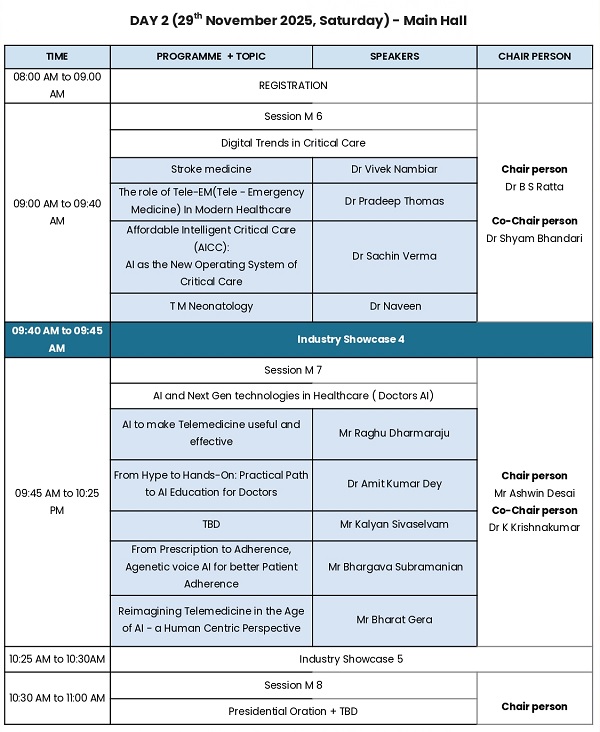
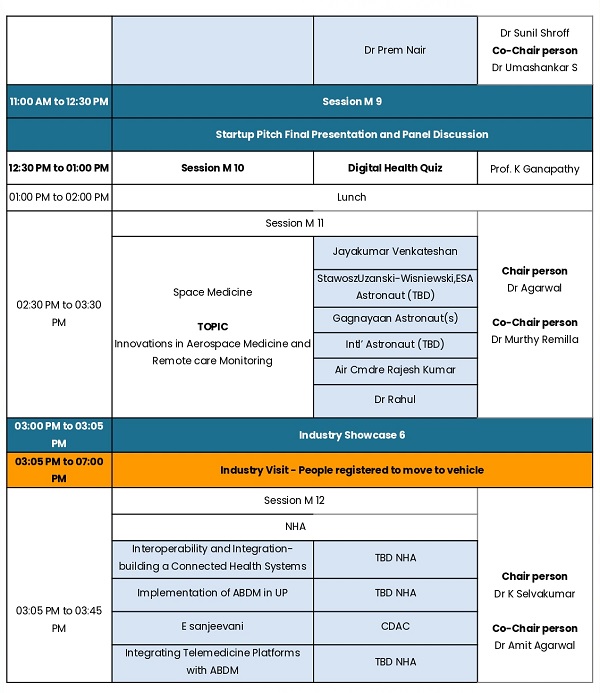
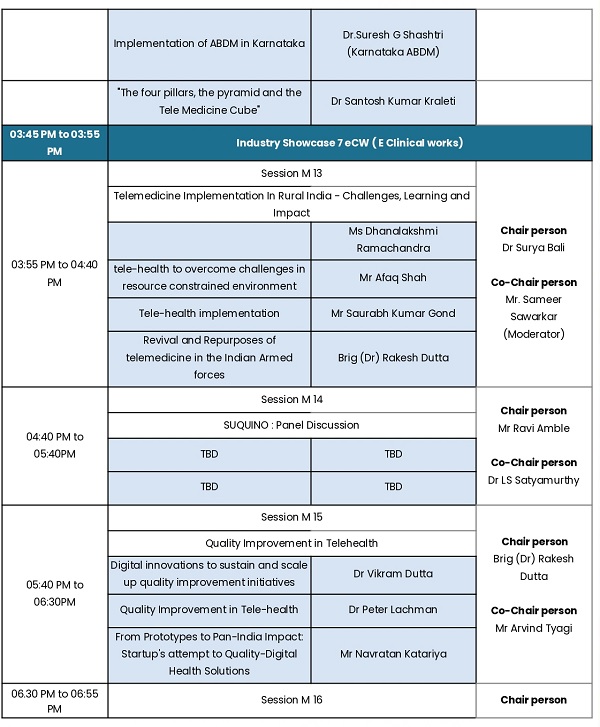
The month of May, however, has otherwise been relatively quiet with limited activities and events. Nevertheless, the focus continues on building capacity, strengthening collaborations, and planning upcoming TELEMEDICON2026 in Jaipur. Registration is now open and I do hope you will avail the early bird registration option .
Thank You
Dr. Sunil Shroff
Chief Editor
President, TSI

Supreme Court Order Signals a Turning Point for Tele-ICU and Digital Health in India
Dr. Sunil Shroff
President, Telemedicine Society of India | Consultant Urologist & Transplant Surgeon
India’s healthcare system may be on the verge of a major transformation following the recent Supreme Court order on ICU infrastructure and critical care preparedness. While the judgment primarily addresses deficiencies in Intensive Care Unit (ICU) facilities, its larger significance lies in the Court’s strong endorsement of tele-ICU systems, digital coordination, GPS-enabled healthcare networking, and technology-driven emergency care.
For the digital health ecosystem, this is perhaps one of the clearest judicial recognitions that technology is no longer optional in healthcare delivery — it is essential. Beyond Bricks and Mortar: The Need for Digital Critical Care
India faces a severe shortage of intensivists, trained critical care personnel, and advanced ICU facilities, especially outside metropolitan cities. Building physical ICUs alone will not solve the problem. Even if infrastructure expands rapidly, specialist expertise cannot be distributed evenly across thousands of hospitals overnight.
This is where tele-ICU systems become transformative.
Tele-ICU models enable specialists located in tertiary centres to remotely monitor, guide, and support healthcare teams in peripheral hospitals through audio-video links, real-time patient monitoring, and digital data sharing. A critically ill patient in a district hospital can effectively receive expert input from a specialist located hundreds of kilometres away.
The Supreme Court’s explicit endorsement of tele-consultation and tele-ICU systems is therefore highly significant. The Court recognized that such systems can reduce unnecessary patient transfers, improve stabilization of critically ill patients, and provide immediate access to specialist advice during emergencies.
A National GPS-Enabled Healthcare Grid
One of the most forward-looking aspects of the order is the direction to explore a nationwide GPS-based digital platform mapping healthcare facilities and ICU availability across India.
Such a system could fundamentally change emergency healthcare delivery.
Today, families often spend precious hours searching for available ICU beds, ventilators, or specialist facilities. Ambulances move from one hospital to another without centralized coordination. Information gaps frequently delay treatment during the “golden hour” of emergency care.
A real-time digital health grid could address these inefficiencies by:
Mapping ICU bed availability
Identifying hospitals with ventilator support
Displaying facility levels and specialist services
Enabling inter-hospital referrals
Coordinating emergency patient transfers
Supporting tele-consultation between institutions
Importantly, the Court emphasized that hospital coordination should happen institutionally and digitally, rather than leaving distressed family members to navigate the system themselves.
Digital Health Infrastructure is Public Health Infrastructure
The order reflects an important shift in thinking. Digital infrastructure is increasingly being recognized as core healthcare infrastructure.
Over the last decade, India has made significant progress in digital public infrastructure through initiatives such as Aadhaar, UPI, CoWIN, Ayushman Bharat Digital Mission (ABDM), and eSanjeevani telemedicine services. However, critical care integration has remained fragmented.
The Supreme Court’s observations could accelerate:
National interoperability standards
ICU data integration
Real-time bed management systems
Emergency response dashboards
Telemedicine integration into routine hospital workflows
AI-supported triaging and monitoring systems
Such integration could become especially valuable during pandemics, disasters, road traffic emergencies, and mass casualty events.
Telemedicine Must Move from Pilot to Policy
India already has successful examples of telemedicine and tele-ICU programmes in government and private sectors. Yet most initiatives remain isolated pilots rather than integrated national systems.
The Court’s endorsement provides an opportunity to move tele-ICU from experimentation to mainstream policy implementation.
For this to succeed, several areas require attention:
Reliable broadband connectivity for hospitals
Standardized tele-ICU protocols
Cybersecurity and patient data protection
Workforce training
Reimbursement and funding mechanisms
Integration with ABDM digital health records
Importantly, tele-ICU systems should complement — not replace — physical critical care infrastructure.
A Vision for Connected Critical Care
The Supreme Court order is more than a healthcare directive; it is a blueprint for connected critical care in India.
The future ICU may no longer be confined within the walls of a single hospital. Instead, India could move towards a digitally networked ecosystem where expertise travels faster than patients, where ambulances become mobile critical care units, and where technology helps bridge the vast urban-rural healthcare divide.
For the digital health community, this order is both a validation and a call to action. The challenge now lies not in recognizing the importance of telemedicine and digital coordination, but in implementing them at scale with urgency, equity, and sustainability.

Reflections from the National Consultative Meeting on Digital Technologies for Mental Health: Evolving Policy and Regulatory Recommendations for Safe Use
Smriti Joshi
Chief of Clinical Services & Ops
Member Board of Directors, Wysa
15–17 April 2026 | Bengaluru
I had the opportunity to participate as an invited expert at the National Consultative Meeting on Digital Technologies for Mental Health: Evolving Policy and Regulatory Recommendations for Safe Use, convened by the NIMHANS–ICMR Centre for Advanced Research in Digital Interventions for Mental Healthcare (NIMHANS–ICMR CAR-DIMH).
The consultation brought together 126 participants from diverse backgrounds—mental health professionals, technology experts, researchers, developers, public health specialists, policymakers, educators, civil society organisations, and representatives from multiple ministries and agencies. What made the meeting particularly valuable was that conversations moved beyond disciplinary silos and focused on a shared question: how do we build digital mental health systems that are useful, safe, and realistic for the Indian context? Digital technologies are increasingly being positioned as one way to address longstanding gaps in mental healthcare—particularly workforce shortages, uneven access to services, stigma, and increasing demand. However, alongside rapid growth in digital mental health applications, important concerns around safety, evidence, privacy, accountability, and implementation are also becoming more visible.
Digital technologies should support care—not replace it
Across discussions, there was considerable agreement that digital mental health tools should strengthen existing systems rather than function independently of them. Participants discussed the potential role of digital tools in improving access, supporting continuity of care, psychoeducation, self-management, and earlier help-seeking, while recognising that technology alone cannot solve structural challenges in mental healthcare.
AI generated both enthusiasm and caution
Conversations explored opportunities around improving access, reducing administrative burden, and supporting clinical workflows, while also raising concerns around emotional dependency, misinformation, overreliance, privacy, and limitations in responding to complex psychological needs.
Governance and safeguards emerged as central concerns
Participants highlighted the need for stronger safeguards around transparency, privacy, crisis response mechanisms, evidence, and accountability.
Recommendations Emerging from Discussions
Develop risk-based governance approaches for digital mental health technologies
Strengthen quality, transparency, and safety standards
Build digital mental health literacy among providers and users
Prioritize responsible digital use among children and adolescents
Strengthen evidence generation and implementation research
For readers interested in exploring the consultation proceedings, stakeholder-specific guidelines, and policy recommendations in greater detail, the following resources are available:
Consultation Proceedings: View Proceedings PDF
Guidelines and Policy Recommendations: View Guidelines PDF
Why These Conversations Matter
For those working in telemedicine, digital health, and healthcare delivery, the discussion increasingly shifts from whether digital mental health technologies should be used toward how they can be implemented responsibly, integrated into existing systems, and evaluated meaningfully.
Rijuven Medicare Wins AP MedTech Innovation Challenge 2026
Uma Mahesh
Vice President – Rijuven Medicare India Pvt Ltd
Treasurer – Telangana State Chapter, TSI
EC Member – National TSI
Rijuven Medicare India Pvt Ltd emerged as the winner in the Remote Patient Monitoring & Telemedicine category at the prestigious AP MedTech Innovation Challenge 2026, a pioneering state-led initiative launched by the Government of Andhra Pradesh to pilot and scale AI-driven healthcare technologies within the public healthcare ecosystem.
Spearheaded by Andhra Pradesh Chief Minister N. Chandrababu Naidu and Health Minister Shri Y. Satya Kumar Yadav, the initiative marks the first time in India that multiple startups have simultaneously piloted AI-enabled healthcare solutions across state-run hospitals.
The AP MedTech Innovation Challenge was launched in November 2025 in association with the Ratan Tata Innovation Hub. A total of 297 startup applications were received, of which 18 innovators were shortlisted through a rigorous multi-stage evaluation process.
The selection process focused not only on technological innovation, but also on real-world healthcare impact and deployability within the government healthcare system. Proposals were screened by the Committee for Applied Technologies in Health (CATH), with scientific and clinical validation support from the Indian Council of Medical Research (ICMR) and the Indian Institute of Science (IISc).
As part of the challenge, participating startups deployed 40 distinct medical devices across 18 Government General and District Hospitals in Andhra Pradesh. Within just 37 days, more than 12,000 patients were screened, significantly improving diagnostic speed and clinical accuracy.
Speaking at the valedictory session held at Mangalagiri, Andhra Pradesh Health Minister Shri Satya Kumar Yadav stated that Andhra Pradesh has become the country’s first “Lighthouse State” in implementing Artificial Intelligence-based healthcare services through the MedTech Challenge.
About Rijuven
Rijuven (India & USA) is a medical innovation company focused on transforming grassroots healthcare delivery through patented healthcare technologies. Its flagship “Clinic in a Bag” solution is designed to modernize healthcare delivery in both rural and urban settings by enhancing capacity, efficiency, accessibility, and outreach.
The solution aims to strengthen primary healthcare services for both communicable and non-communicable diseases, enabling healthcare providers to reach and serve millions more effectively.
Rijuven expressed pride in being selected among the 18 finalists for pilot implementation under the AP MedTech Innovation Challenge and described the recognition as a significant milestone for the organization.
The company conveyed its gratitude to the Government of Andhra Pradesh, Hon’ble Health Minister Shri Satya Kumar Yadav, the GGH Kurnool team, evaluators, clinical teams, mentors, and supporters who contributed to the success of the initiative.
Special thanks were also extended to mentors and well-wishers at the Telemedicine Society of India (TSI) for their continued guidance and encouragement throughout the journey.


“Pilgrimage Telemedicine”
Dr Nitha V Panicker
Secretary, TSI Kerala Chapter
The Kerala Kumbh Mela, held on the banks of the Bharathapuzha River (Nila) at Thirunavaya, in Malappuram district, is a centuries-old sacred congregation widely revered as the “Kumbh of the South.” Rooted in holy river bathing, Vedic rituals, ancestral worship, and spiritual traditions, this historic Maholsavam was conducted from January 18 to February 3, 2026, witnessing the participation of approximately 4–5 lakh pilgrims. The event featured sacred immersions, traditional rituals, and the Nila Aarti, making it one of the largest and most spiritually significant religious congregations in South India, symbolizing Kerala’s deep-rooted cultural and spiritual heritage.
As part of this historic gathering, a comprehensive Pilgrimage Telemedicine Programme was implemented to ensure accessible, timely, and quality healthcare services for pilgrims. The programme was organized in association with Mata Amritanandamayi Math, Juna Akhada, Amrita Institute of Medical Sciences, the Amrita Telemedicine Unit, and the Telemedicine Society of India – Kerala Chapter. This “Pilgrimage Telemedicine” facility was inaugurated by Kummanam Rajasekharan, Former Governor of Mizoram, along with Dr. Jaggu Swami Hospital Administrator, AIMS, Swamini Athulyamrita Praana (Mata Amritanandamayi Math Thirur), Brahmachari Pramod MA Math Haridwar , Dr. Sreekumar C (Professor of General Surgery & Telemedicine Medical Officer), and Mr. Rajeesh M. V (Telemedicine System Administrator), marking a significant milestone in integrating spiritual pilgrimage with modern digital healthcare systems.
Through advanced telemedicine infrastructure, Thirunavaya and Tavanur were digitally connected to Kochi, enabling pilgrims to receive direct expert medical guidance from Amrita Hospital through real-time teleconsultations. More than 400 pilgrims benefited from these services, receiving specialist consultations, clinical guidance, and timely medical support without the need for physical hospital travel. This initiative stands as a landmark model of faith–healthcare integration, demonstrating how digital health technologies can effectively support large-scale pilgrimage events by ensuring accessibility, and quality healthcare delivery while preserving the spiritual sanctity of the sacred gathering.



Why Over 66 Million Americans Use AI for Healthcare
Manjubashini
M.Sc (Bio-Informatics)
Content Writer, Medindia.net
The rise of AI-driven healthcare is transforming the American medical landscape. A landmark April 2026 West Health-Gallup study reveals that 66 million U.S. adults now consult AI chatbots for medical advice.
Rather than replacing doctors, most patients use generative AI to supplement visits, researching symptoms before appointments or interpreting diagnosis data afterward. However, 14 million Americans have used AI as a substitute for professional care, driven by high healthcare costs and accessibility barriers.
Despite this trend, trust remains low, with many reporting concerns over medical accuracy and safety. For providers, this digital shift highlights an urgent need to integrate AI tools into patient workflows to ensure responsible, guided health outcomes.
Enhancing Patient Confidence: The Role of AI in Pre- and Post-Visit Care
The study shows how AI tools act as a digital bridge between patients and providers. By leveraging chatbots for pre-visit symptom checks and post-visit data interpretation, users gain the confidence and clarity needed to navigate complex clinical conversations, making care more collaborative.
Before the visit: 59% of patients use AI to research symptoms so they can ask better questions.
After the visit: 56% of patients use AI to interpret medical jargon or get more details on a diagnosis.
For Confidence: 46% of users say AI makes them feel more confident when talking to their healthcare provider.
AI Chatbots as an Essential Alternative for Cost-Effective Healthcare Access
While AI primarily serves as a support tool, it is increasingly becoming a vital source for those facing healthcare structural barriers. For many people, chatbots are not just a choice but an essential alternative driven by high costs and limited access.
This shift highlights a growing socioeconomic divide, where AI fills the gap for underserved populations who feel marginalized or excluded from traditional clinical care. While most use it as a supplement, a smaller but significant group is using AI as a substitute:
Avoidance: About 14% of people (roughly 14 million people) decided not to see a doctor specifically because of the guidance they received from AI that makes them potentially substitute professional consultation.
Barriers: While 27% of people turn to AI tools over doctors primarily due to cost, 21% of people use AI due to lack of time, or past negative experiences where they felt dismissed by human doctors (21%).
Income Gap: There is a sharp economic divide; 32% of lower-income users used AI because they couldn’t afford a doctor, compared to only 2% of high-income users.
High Usage vs. Low Trust: The Trust Deficit in AI Medical Accuracy
According to the West Health-Gallup data, the paradox of AI healthcare lies in the trust gap. Despite widespread use, skepticism remains high, with many users questioning the accuracy of AI’s information, 11% of users are flagging safety risks, a trend that indicates a critical need for oversight.
Despite the high usage, trust in AI’s medical accuracy is surprisingly low as follows:
Divided Trust: Only 33% of users say they actually trust the information they receive from AI; and the rest are neutral or distrustful.
Strong Trust: Only 4% of users strongly trust the health information accuracy of these AI tools.
Safety Risks: 11% of users reported that AI gave them medical advice they believed was unsafe.
How AI Drives Wellness Tracking and Medication Research
AI tools are now a common first point of contact for healthcare management, providing immediate access to medical information. From tracking daily wellness habits to identifying physical symptoms and researching medication risks, these platforms offer real-time data that helps users monitor and manage their health more independently.
The most frequent reasons for consulting AI tools include:
Nutrition and exercise (59%): Most common for lifestyle and wellness guidance.
Physical symptoms (58%): Used frequently for preliminary symptom-checking.
Medication side effects (46%): Helps users understand pharmaceutical risks and interactions.
Mental health concerns (24%): Provides a private avenue for emotional and psychological support.
Evidence-Based Oversight: Global AI Frameworks and Safety Standards
To bridge the gap between AI utility and clinical safety, global healthcare systems are implementing rigorous oversight. Beyond user trends, new regulatory frameworks and institutional case studies demonstrate a shift toward standardized, transparent, and legally accountable AI integration in healthcare.
As of January 1, 2026, several major U.S. states have enacted laws specifically to address the risks of AI in clinical settings:
The most direct law of California ‘AB489’ prohibits AI developers from pretending to be a doctor. Systems cannot use any design elements, phrases, or titles that imply the AI holds a medical license.
The ‘Texas Responsible Artificial Intelligence Governance Act (TRAIGA)’ law requires conspicuous written disclosure from physicians. Doctors must tell patients if they are using AI for diagnosis or treatment. If they don’t, they face fines up to $200,000 per violation.
For mental health or wellness chatbots, California now mandates crisis protocols ‘Safety Protocols (SB 243).’ According to this law, if a user mentions self-harm, the AI is legally required to immediately stop and provide a referral to a human crisis provider or operator’s internet website.
Universal Regulatory Initiatives and Clinical Integration of Healthcare AI
On a global scale, the Organization for Economic Co-operation and Development (OECD’s) 2026 framework, ‘Scaling AI in Health,’ introduces international standards for ‘Model Cards.’ The model cards are digital transparency labels that detail an AI’s training data, limitations, and accuracy.
These transparency labels certify that AI tools are trained on data representing diverse populations, ensuring equitable care. By setting these benchmarks, the OECD aims to standardize clinical safety and data integrity, transforming AI from a localized tool into a globally regulated health resource.
Professional healthcare systems are now countering public chatbots with validated AI integrated into official workflows. At the American Medical Group Association (AMGA) 2026 Annual Conference, clinical leaders presented ‘Ana in Action,’ a study on using automated AI assistants to reduce administrative burden. This approach maintains patient-centric oversight, ensuring AI acts as a clinical support tool rather than a standalone replacement.
India’s Press Information Bureau (PIB) recently launched the Strategy for Artificial Intelligence in Healthcare for India (SAHI), a national framework focusing on trust, diversity, and inclusion. The mandate prioritizes localized datasets to ensure AI algorithms are representative of India’s unique demographics, while establishing ethical oversight to strengthen public confidence in digital health.
The Future of Healthcare: Balancing AI Innovation with Patient Safety
The West Health-Gallup study confirms AI is reshaping healthcare as a vital support tool. While improving accessibility, its rise highlights urgent needs for medical accuracy and safety. Moving forward, health systems must prioritize ethical integration and clinical oversight.
Ultimately, AI should bridge equity gaps and enhance care, serving as a supportive resource rather than a replacement for professional medical consultation.

Is Telehealth Reliable for Autism Diagnosis?
Adeline Dorcas
M.Sc, M.Phil (Food Service Management & Dietetics)
Content Writer, Medindia.net
Is telehealth good enough for autism diagnosis? Yes, autism diagnosis has gone virtual and proven to be pretty effective during the COVID-19 pandemic, according to a new study.
Pandemic Pause: Autism Diagnoses Put on Hold by COVID-19
When the COVID-19 pandemic led to clinic closures and limited in-person interactions to masked encounters, autism diagnoses for many children were put on hold.
For Katherine Meltzoff, a professor of education at UC Riverside, the disruption exposed a critical gap and an opportunity.
“We were trying to figure out how to adapt autism diagnostics to be done virtually,” Meltzoff said. Telehealth Takes the Lead in Autism Detection Amid COVID-19
The result is a set of telehealth tools described in a paper published in the Journal of Autism and Developmental Disorders that are designed to help clinicians diagnose autism remotely, especially for children who are older or have developed verbal communication skills.
Telehealth’s Growing Role in Autism Care
Meltzoff explained that there are already a number of validated virtual autism assessment tools for children aged 3 and below, and for those with minimal spoken language, but not for those who are older and have more verbal speech.
“Telehealth seems to work really well for the kids that have more obvious symptoms and that are younger,” said Meltzoo, the lead author.
Meltzoff’s research tested whether these virtual assessments could match the accuracy of traditional, in-person evaluations, offering a potential solution to long-standing barriers in autism diagnosis.
More Than Tests: Diagnosing Autism Through Behavior
Autism spectrum disorder is not diagnosed through a single medical test. Clinicians observe how a child communicates, interacts socially, and responds to the world, while also reviewing developmental history.
“We diagnose it behaviorally, so we’re looking at behaviors that the child displays,” Meltzoff explained.
Lost Expressions Behind the Mask: The Challenge of Autism Evaluation During COVID-19
During the first months of the COVID-19 pandemic, autism assessments came to a halt due to the widespread ‘shelter at home’ guidelines. As restrictions began to ease, assessments remained challenging because facemasks worn by the clinicians and family members hid facial expressions, which are a large part of the social communication and behaviors under evaluation.
In traditional clinical settings, those observations happen during carefully structured, in-person sessions. For her study, Meltzoff recreated those interactions online. Using video conferencing tools, clinicians guided parents through activities — such as calling a child’s name or engaging in play — while observing how the child responded. For older children, clinicians interacted directly with them through conversation and structured tasks.
A Tale of Two Assessments: Telehealth vs. In-Person Autism Diagnosis
To test accuracy, Meltzoff and her team recruited 39 children seeking autism evaluations through a university-based clinic. Each child underwent two separate assessments — one in-person and one via telehealth — conducted by different clinical teams who were unaware of each other’s conclusions.
The results were promising. One of the tools developed for children whose speech is limited to short phrases showed particularly high accuracy, while another designed for more verbally fluent children was effective in many cases but less consistent.
The study also found that parents were largely satisfied with telehealth assessments, suggesting the approach is both feasible and acceptable for families.
The need for alternatives to in-person diagnosis is significant, Meltzoff said.
“A lot of people live two hours from an autism clinic,” she said. “Getting your kid two hours to a clinic, then doing an appointment and two hours home just isn’t really feasible.”
The approach is especially important for families in rural areas or those with limited financial resources. For some, transportation costs or lack of access to reliable transit can make in-person visits difficult.
Speech Therapy, Occupational Therapy, and Behavioral Therapy: Supporting Child Development in Autism
Additionally, a formal autism diagnosis is often required to access essential services. While schools can provide some support without a clinical diagnosis, insurance coverage for therapies typically depends on one. Those services include speech therapy, occupational therapy, and one-on-one behavioral interventions — all of which can be critical for helping children develop communication and life skills.
Still, Meltzoff cautions that telehealth is not a one-size-fits-all solution. Children with more subtle symptoms or co-occurring conditions such as attention deficit and hyperactivity disorder (ADHD) may still require in-person evaluations for accurate diagnosis.
“I don’t want to oversell it,” Meltzoff said. “It worked for most kids, but more complex cases — the ones that are already difficult even when done in-person — can be harder to evaluate remotely.”
Even with those limitations, the study validates new tools for children with a wider range of communication abilities.
“How accurate is telehealth?” Meltzoff asked rhetorically. “We found it’s pretty good.”
::ANNOUNCEMENTS::
TSI Executive Committee Election Result
The Telemedicine Society of India (TSI) conducted elections for the vacant post of Executive Committee Member for the term 2025–2027. As only one valid nomination was received, Dr. Amit Aggarwal (LM0338) was elected unopposed as Executive Committee Member.
The election process was conducted under the supervision of Dr. Murthy Remilla, President-Elect & Returning Officer, TSI.
New Life Members Joined – April & May 2026
TSI is pleased to welcome the following new Life Members who joined during April and May 2026:
Dr. Gopal Shah (Gujarat)
Dr. Nikhil Mehta (Chandigarh)
Dr. Parmar Kinjal Jashubhai (Gujarat)
Dr. Hetal Vadiwala (Gujarat)
Dr. Jagdish Sakhiya (Gujarat)
Dr. Subash Chandra Sarangi (Odisha)
Prof. Shabir A. Sofi (Jammu & Kashmir)
Dr. Subrata Kumar Datt (Karnataka)
New Paramedic Members Joined – April 2026
TSI warmly welcomes the following new Paramedic Members who joined in April 2026:
Mr. Sharvan Kumar (Punjab) and Mr. Ramandeep Singh (Punjab).
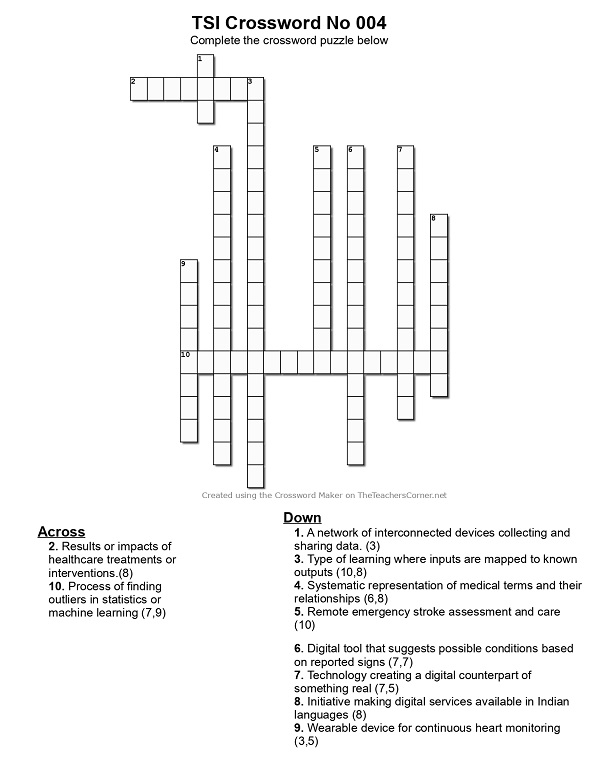
::CROSSWORD::

Click here to Print the Crossword
Click here to view the Crossword Rules and Regulations
Compiled by Dr.Umashankar
Answers in June 2026 Newsletter!
Telemedicine – News from India & Abroad
Why NHS Plans to Use AI to Reduce Healthcare Staffing Costs
Could AI help the NHS avoid financial ruin as Britain plans to slow healthcare recruitment and automate admin work?…………….. Read More
AI Systems Pass the Turing Test: What This Means for the Future
Understanding the impact and implications of AI systems designed to mimic human behavior and decision-making…………………. Read More
Telemedicine Practice Guidelines – A Foundation Course for RMPs by TSI Faculty
To know more about the Telemedicine Foundation Course click on the link below:
https://tsitn.org/tpg-course/
Medical Writing Certificate Course with Internship Opportunity!
TSI invites all the TSI Chapters and Members to submit information on their upcoming Webinar or Events (50 words), News related to Telemedicine (200 words) or short articles (500 words) for the monthly e-newsletter.Guidelines for submission to TSI Newsletter-
- Report can be from 500 to 600 words
- Report Should be relevant to Telemedicine or Medical Informatics
- No promotion of self or any product
- Avoid plagiarism
- All references should be included
- Provide any attributions
- Visuals are welcome including video links
- Send full authors name, degrees, affiliations along with a passport sized photograph of good resolution. If multiple authors only main author photo to be sent.
Submission may be sent to – tsigrouptn@gmail.com
Editors reserve the rights for accepting and publishing any submitted material.
Editor in Chief – Dr. Sunil Shroff
Editors – Dr. Senthil Tamilarasan & Dr. Sheila John
Technical Partner- https://www.medindia.net