Click Here to Download PDF Version
Telehealth Newsletter
Official Newsletter of Tamil Nadu Chapter of Telemedicine Society of India
|
What is New? The month of August issue has three interesting articles. The first is from Anay on consultations between two doctors, relating to the care of a patient, as telemedicine consultations and the legal requirements. The second is from Prof Ganapathy about having a band of clinician scientists and clinical technologists to help with growth of telehealth. He also emphasizes the role of clinical research. Teladoc has been in the news and we bring you the experience on how these telemedicine robots have the capabilities to carryout basic clinical examination (such as checking blood pressure and heart rate) on their own, as instructed by the doctors. At Meenakshi Mission, these robots have empowered the doctors to treat patients anywhere and anytime. Thank You |
 Teleconsultations between doctors
Teleconsultations between doctors
Mr. Anay Shukla
Founding Partner, Arogya Legal – Health Laws Specialist Law Firm
Ms. Eshika Phadke
Associate, Arogya Legal – Health Laws Specialist Law Firm
Telemedicine, as a practice, is typically associated with consultations that take place remotely between a doctor and a patient. While doctors are familiar with the Telemedicine Practice Guidelines, 2020(“Telemedicine Guidelines”) and its applicability to such consultations. However, it should be noted that the Telemedicine Guidelines has adopted a broader interpretation of what amounts to a teleconsultation, and classifies consultations between two doctors, relating to the care of a patient, as telemedicine consultations.
In practice, a doctor (“treating doctor”) may often need to consult with another doctor (“consulting doctor”) to determine the best course of treatment for a patient. For example, while consulting with a professional of another specialty or with extensive experience in treating a certain condition. Such consultations would generally take place when the patient is physically present with the treating doctor, but there is no bar on all three participants consulting remotely.
The mechanism for such consultations is largely similar to traditional teleconsultations between a patient and doctor. However, there are certain considerations that a doctor should be mindful of while engaging in a consultation involving another doctor.
Explicit Consent
The general principle is that when a patient initiates a teleconsultation with a doctor, their consent is implied. However, in case of a consultation between two doctors and the patient, even if the patient has initiated the consultation, it is best to obtain explicit consent from the patient for the consultation with both doctors.
In the event that the treating doctor initiates the consultation, explicit consent is required to be sought from the patient prior to proceeding with the consultation. Such consent may be obtained through a text message, email or voice recording, or the doctors may have the patient categorically confirm that he/she consents, and record the same. As a matter of practice, both the treating doctor and the consulting doctor should record the consent in their notes.
The treating doctor should also obtain explicit consent from the patient before sharing information or records with the consulting doctor, even if the patient has consented to the consultation.
Patient History
The consulting doctor may rely on the information provided by the treating doctor, including their findings in a physical examination. In addition, the consulting doctor may gather additional information from the patient, as they deem fit. The consulting doctor may recommend to the treating doctor that certain additional tests be carried out if required.
Control of case
As per the Indian Medical Council (Professional conduct, Etiquette and Ethics) Regulations, 2002 (“Code of Ethics”) the consulting physician is required to discuss the diagnosis treatment plan with the treating doctor, and should not take charge of the case.
In case of a consultation involving two doctors, the consulting doctor should be mindful that the case has not been handed over to them, and that the ultimate control rests with the treating doctor. The treating doctor must exercise professional discretion and determine how to proceed with the patient’s care.
While recommending a treatment plan, the consulting doctor should be mindful of the restrictions, if any, that the treating doctor may be subjected to. For example, if the treating doctor does not have the training to administer a treatment or procedure, the consulting doctor should clarify that the patient would need to seek such treatment from another professional. However, in doing so, the consulting doctor should be careful to not professionally undermine the treating the doctor or his treatment plan.
 Necessity for formally dually trained Clinician Scientists and Clinician Technologists
Necessity for formally dually trained Clinician Scientists and Clinician Technologists
Prof. K. Ganapathy
Past President, Telemedicine Society of India & Neurological Society of India | Hon Distinguished Professor The Tamilnadu Dr. MGR Medical University | Emeritus Professor, National Academy of Medical Sciences | Formerly Adjunct Professor IIT Madras & Anna University | Director Apollo Telemedicine Networking Foundation & Apollo Tele Health Services | URL: www.kganapathy.in
Healthcare necessitates bridging the gap between full time clinicians, full time medical researchers and full time engineers and technologists working in Healthcare. I have pioneered Stereotactic radiosurgery in 1995 and have always been interested in the use of Technology in Healthcare. In the article that has a link provided, I speak about the relevance in emerging economies and strongly supports the plan to create a band of clinician scientists and clinician technologists. This will also ultimately help the growth of Telehealth. The article is available at:https://issuu.com/verticaltalk/docs/ahhm-issue-57/20

2. RELEVANCE OF CLINICAL RESEARCH
The growth and development of any discipline or area ultimately depends on providing unequivocal scientific evidence that a particular facility / intervention in this case Telehealth (Remote Health Care) has indeed made a significant difference. Unfortunately in the real world priorities for clinical research takes a back seat. In this presentation I share “Lessons learnt & Opportunities missed: over 54 years in Clinical Research”. Hopefully the present generation with all the technology at its command will not only evangelise Telehealth but equally important produce hard core irrefutable evidence that telehealth needs to be incorporated into the mainstream of Healthcare.
 Mobile Teladoc Health Robots at MMHRC
Mobile Teladoc Health Robots at MMHRC
Mr. P. Sundarraj
Head – R & D, Meenakshi Mission Hospital and Research Centre, Madurai
In India, despite several advancements made in the medical field, the benefits are still available to the privileged who are residing mainly in the urban areas. It is known fact that 75 percent of the qualified doctors practice in urban centres, whereas the vast majority of India’s population live in the rural areas. To address the issue, Meenakshi Mission Hospital and Research centre in Madurai extends its support by establishing Telecare centres in remote rural areas. So far it is established 15 centres in and around southern Tamilnadu with the support of public undertaking sectors & corporate.
To bridge the health and technology intensively, MMHRC gone for next phase and establish India’s first telehealth robots.
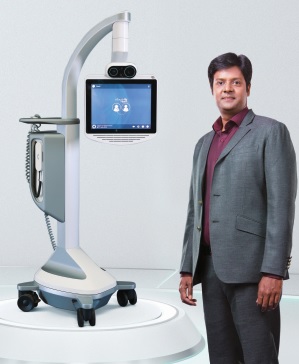
First of its kind in India, Meenakshi Mission Hospital and Research Centre have deployed 16 mobile Teladoc (USA) health robots. The primary objective of the Teladoc robot is to argument the diagnostic abilities and efficiency of health care delivery of patients irrespective of their physical location.
The Teladoc telemedicine robots have the capabilities to carry out basic clinical examination (such as checking blood pressure and heart rate) on their own, as instructed by the doctors. As 10T devices, they can be used to control other advanced diagnostic equipment such as CT and MRI scan machine. These robots can collect and process data from other diagnostic equipment and present it to doctors to help them make precise clinical questions with the help of Teladoc, doctors from different disciplines, from all parts of the world, can come together to treat and monitor patients all the time.
At Meenakshi Mission, these robots have empowered our doctors to treat patients anywhere and anytime. Our ambulances will also be equipped with Teladoc robots. By doing this, the patient can immediately get in touch with the emergency and ICU specialists along with the other specialists of all departments. This means that specialists like neurologists and cardiologists can begin vital treatment even as critically all patients are on their way to the hospital.
We are all set to explore ways to use this novel technology to provide expert diagnosis from Madurai to patients in other parts of the country and put world class health care with in every ones reach.
Telemedicine – News from India & Abroad
Can Artificial Intelligence Detect Autism Early?
Artificial intelligence (AI) can soon be used to detect autism spectrum disorder (ASD) early, reveal researchers at the University of Arkansas.Han-Seok Seo, an associate professor with a joint appointment in food science…..Readmore
AI Algorithm Helps Cure Epilepsy
An artificial intelligence (AI) algorithm developed by researchers detects subtle brain abnormalities which cause epileptic seizures.The Multicentre Epilepsy Lesion Detection project (MELD) used over 1,000 patient…Readmore
New Stamp-sized Ultrasound Stickers can Monitor Your Internal Organs
New stamp-sized ultrasound sticker has been developed by a team of engineers in the US. The device can stick to skin and can provide continuous ultrasound imaging of internal organs for 48 hours….. Readmore
Can Artificial Intelligence Improve Stroke Diagnostics?
Artificial intelligence (AI) technology identifies when a patient is having a stroke caused by emergent large vessel occlusion (LVO), therefore making them a candidate for endovascular therapy (EVT)….Readmore
Click here to Become a Member of Telemedicine Society of India
Telemedicine Practice Guidelines – A Foundation Course for RMPs by TSI Faculty
To know more about the Telemedicine Foundation Course click on the link below:
https://tsitn.org/tpg-course/
TN – TSI invites all the TSI Chapters and Members to submit information on their upcoming Webinar or Events (50 words), News related to Telemedicine (200 words) or short articles (500 words) for the monthly e-newsletter.Guidelines for submission to TN TSI Newsletter-
|
Submission may be sent to – tsigrouptn@gmail.com
Editors reserve the rights for accepting and publishing any submitted material.
Editor in Chief – Dr. Sunil Shroff
Editors – Dr. Senthil Tamilarasan & Dr. Sheila John
Technical Partner- https://www.medindia.net



