Telehealth Newsletter
Official Newsletter of Telemedicine Society of India

What is New?
The latest news is the shift of TELEMEDICON 2024 from Dharamsala to Chandigarh, to be conducted from 28th to 30th Nov 2024.
This last minute decision was made after much deliberation and discussion. Several issues arose with this remote location selection for a national conference without adequate due diligence. Access to Dharamsala was difficult with skyrocketing airfares, and many members expressed their inability to attend. Additionally, there was a lack of understanding and cooperation on how the conference would be coordinated locally by the Himachal chapter between two major institutions.
Post elections, we had the Budget 2024-25 announcement. And in this healthcare allocation has been almost ₹90,000 crores, with notable inclusions for telemedicine. Under the tertiary care program, funds are transferred to states for implementing various schemes, including:
- Tobacco Control and Drug De-addiction Control Programme
- National Mental Health Programme
- Assistance for Capacity Building for Trauma Centres
- National Programme for Prevention and Control of Cancer, Diabetes, Cardiovascular Diseases, and Stroke
- Health Care for the Elderly
- National Programme for Blindness
- Telemedicine
This segment saw an increase in budgetary allocation from ₹276 crores to ₹369 crores.
The National Tele Mental Health Programme aims to provide universal access to equitable, accessible, affordable, and quality mental health care through 24×7 tele-mental health counseling services. As a digital component of the National Mental Health Programme (NMHP), it covers all Indian states and UTs with assured linkages and received a budgetary allocation of ₹90 crores.
So book your tickets for Chandigarh in advance and start preparing your abstracts!
Thank You
Dr. Sunil Shroff
Chief Editor
Vice President, TSI
::ANNOUNCEMENTS::

::Education Section::

Doctor-Patient Relationship in Tech-enabled Healthcare
Dr. K. Ganapathy
Distinguished Visiting Professor IIT Kanpur | Distinguished Professor The TamilnaduDr MGR Medical University | Emeritus Professor National Academy of Medical Sciences | Past President : Telemedicine Society of India, Neurological Society of India, Indian Society for Stereotactic & Functional Neurosurgery | Formerly WHO Digital Health Expert | Director Apollo Telemedicine Networking Foundation & Apollo Tele Health Services
1968 : I entered Medical School 56 years ago. Trained in the 20th century, in the BC era my generation would today be considered to belong to the Neanderthal Age.
I injected air into the brain and dyed directly into the Carotid Artery to see if there was any displacement of ventricles or blood vessels in the brain – a surrogate marker for a possible “Space Occupying Lesion”. Tuberculoma and Cysticercosis (growths due to TB and parasites) were as common as benign and malignant brain tumors. Getting the patient’s consent for surgery was a one-sided conversation.
No questions were asked. Such was the faith and trust reposed in the surgeon. The role of the patient and the family in the decision-making process was minimal. We could not share our responsibility with anyone.
I was Amicus curiae and the Devil’s Advocate rolled into one. We entered the brains of our patients even before the surgery, trying to understand what he/she and their families would want, and took a surrogate decision on their behalf, in their interests.
2024: Tomorrow the Digital Health we will be practicing will be 5P (Predictive, Personalized, Precision, Participatory, and Preventive) medicine with AI as a major component. As 80% of the 41 Zetabytes (410 trillion GB) of digital information currently available is unstructured AI will detect patterns and trends, which our gray matter is unable to decipher.
Powerful AI techniques are unlocking clinically relevant information, hidden in massive amounts of data. Wanting to be future-ready and ahead of the curve, are we turning a Nelson’s eye and forgetting our past?
After all, it is NI (Natural, Native) Intelligence that led to the birth of AI. In a world where algorithms make diagnoses, wearables track vital signs, and robots are remotely controlled, to perform surgical procedures, will clinicians of the last century become an endangered species?
Technology today is working overtime to guarantee patient safety and quality improvement. There is already a marked shift in using technology to promote good health. In the next two decades the necessity to diagnose and treat established diseases will significantly reduce. There will be no chapter on “Complications”.
Genomics, radiomics, and specialties hardly existing today will replace many disciplines. The increasing use of a Digital Twin of a patient will enable accurate assessment and a preliminary “ in silico” trial.
We need to remind ourselves that technology is a means to an end, not an end by itself. Proactive measures need to be taken to ensure that increasing the use of technology does not lead to depersonalization and dehumanization.
Sir William Osler’s observations 150 years ago “ — the good physician treats the disease, the great physician treats the patient who has the disease”
“—–Patients don’t care how much you know until they know how much you care”
“—Listen, listen, listen he is telling you the diagnosis” is even more relevant today. The world has turned upside down. Very soon a clinician who does not use AI in his/ her armamentarium would appear to have come from another planet!
Terms such as “ trust” and TLC (Tender Loving Care) espoused by my teachers, may soon disappear. Once new technologies roll over you, if you are not part of the steamroller, you are part of the road. The writing is on the wall!
The ultimate disruption will be when what today is termed AI will become ANI, not perhaps in my lifetime but certainly in the lifetime of my children.
The A in AI after all stands for Augmenting, Amplifying, Accelerating, Assisting, and Analyzing in an Ambient milieu.
A smart empathetic clinician using ANI will become smarter. A mediocre clinician using ANI will not necessarily become smarter. The Hippocratic Oath may have to be replaced with a Robocratic Oath.
After all “To err is ChatGPT, to forgive is human !!”
Click here to view the Latest daily healthcare news & updates-Digital Health News

TELEPSYCHOLOGY IN DEVELOPMENT: BOUNDARY ISSUES AND RECOMMENDATIONS
Dr. Vikrant Mittal
MBBS, MD (Psychiatry, Yale),
MHA (Johns Hopkins), FACHE, FAPA
Ms. Swati
BA, MA, MPhil (Psychology),
PhD (candidate)
The use of technology-assisted mental health services by both practitioners and clients is increasing significantly so the telepsychology clinicians need to get ready to give competent care in this constantly changing service delivery environment. The “Guidelines for the Practice of Telepsychology” were published by the American Psychological Association in 2013 and, comparable guidelines for therapeutic online work have been published by the British Association for Counselling and Psychotherapy (BACP) in the UK. The aforementioned advancements highlight the growing fascination with virtual therapy among the counselling and psychotherapy fields. They have cleared the path for “telepsychology,” commonly referred to as online therapy, e-therapy, or e-counselling abroad, to gain official recognition.
The human interaction that is essential in a counsellor’s office is merely not feasible through computers or phones (Maples & Han, 2008). Therefore, in a therapeutic relationship, a lack of physical presence can impede the formation of a therapeutic alliance between the therapist and the patient. Misunderstandings can occur more frequently when there are no visual or auditory cues present, such as body language, tone of voice, or facial expressions. This suggests that boundaries are quite important in telepsychology. Counsellors and clients mostly communicate face-to-face through body language, posture, eye contact, and other nonverbal cues. Reading nonverbal cues is undoubtedly a crucial part of counselling. Since these nonverbal cues are invisible when receiving counselling online, their absence may compromise the effectiveness of the session.
Psychologists today are challenged as ethical decision makers by the ever-expanding development and use of digital technology in their own lives and in the lives of their clients. Boundaries are generally helpful from a clinical standpoint because they help clarify the nature of the therapeutic relationship and assist both the client and the clinician in controlling their conduct in a way that optimizes benefits and reduces risks (Borys, 1994). In addition, boundaries can support various other therapeutic goals such as creating a trustworthy working alliance, teaching the client assertiveness techniques, increasing the client’s sense of value (by honoring their autonomy and rights), and maintaining the integrity of the relationship (Borys, 1994; Smith & Fitzpatrick, 1995). Appropriate boundaries shield physicians from damage in addition to protecting the client.
BOUNDARY RELATED ISSUES
Time-related considerations and issues
Time boundary problems are not unusual in traditional in-person therapies; they usually manifest as early or late session arrivals, session extensions, meeting at strange or inappropriate hours, excessive contact outside of sessions, and booking specific clients for the last appointment of the day (Zur, 2007). These problems can definitely arise in telepsychology contexts as well, and they might even be more common because of the medium’s flexibility, the idea that it is convenient for both sides, and the possibility of a less controlled and regulated work environment.
Aspects and problems connected with settings
The adaptability of telepsychology and the capacity to work at any time and from any location offer one difficulty. Because of this flexibility, therapeutic interactions between clients and clinicians may occur in public places. While social interactions in public places might seem harmless at first, they can have serious repercussions. In addition to putting the client’s confidentiality at danger (for example, by using an insecure public internet connection or inadvertently letting others access the therapeutic discussions), the clinician can face legal and professional repercussions for their actions. Apart from jeopardizing the client’s anonymity, this could potentially undermine the therapeutic gains since the surrounding stimuli could operate as distractions and hinder the client’s ability to fully comprehend the therapeutic material.
Considerations and issues specific to the therapist
Boundary difficulties can also develop in other contexts that are unique to the therapist, such as when the therapist faces challenges to their own self-imposed limits, when they are concerned with language and phrase choices, or when they are concerned with safeguarding their work. Regarding obstacles to one’s own personal limits, specialists may find themselves working at hours that they would not ordinarily work due to the flexibility that telepsychology services allow.
RECOMMENDATIONS
Be mindful of the session times and observe professional hours.
Make sure that feedback is given on time and consistently, and their is control over communication.
Establish a Confidential, Uniform, Expert, and Culturally Appropriate Environment.
Protect Non-Clients’ Privacy and Avoid Inadvertent Self-Disclosures.
Make Sure the Technologies Used for Telecommunication Project Professionalism.
Establish Proper Self-Boundaries.
Protect the Therapist’s Work Privacy.
Speak professionally and take into account alternate interpretations.
Assure Competence in Telepsychology Practice
Telemedicine Practice Guidelines, published by the Indian government lately, legitimize teleconsultations. However, there is not much discussion of psychotherapy methods in these guidelines. These evolving psychotherapy delivery technologies will raise an increasing number of moral and legal questions. Concerns regarding the safety of therapists are also raised by the paucity of research documenting instances of harassment experienced by them in virtual environments. Few psychologists are equipped to handle such difficult circumstances since the ethical concerns raised when clients threaten, stalk, or harass their psychotherapists online have typically received little attention in the literature. Thus, both the patient and the therapist will benefit from greater research in this field.
References
Borys, D. S. (1994). Maintaining therapeutic boundaries: The motive is therapeutic effectiveness, not defensive practice. Ethics & Behavior, 4(3), 267-273.
Drum, Katherine B. and Littleton, Heather L. (2014). Therapeutic boundaries in telepsychology: Unique issues and best practice recommendations. Professional Psychology Research and Practice, 45(3); 309-315.
Hudson-Allez, G. (2006). The stalking of psychotherapists by current or former clients: Beware of the insecurely attached!. Psychodynamic Practice, 12(3), 249-260.
Kotera, Y., Kaluzeviciute, G., Lloyd, C., Edwards, A. M., & Ozaki, A. (2021). Qualitative investigation into therapists’ experiences of online therapy: Implications for working clients. International journal of environmental research and public health, 18(19), 10295.
Lokai, A. D., Liqiaonan, C., Terry, K., Eubanks, C. F., & Muran, C. (2021). Transitioning to virtual space: Teletherapy in the time of COVID-19. Psychotherapy Bulletin, 56(2), 29-34.
Maples, M. F., & Han, S. (2008). Cybercounselling in the United States and South Korea: Implications for counselling college students of the millennial generation and the networked generation. Journal of Counselling & Development, 86(2), 178-183.
Mateescu, V. M. (2021). Distance and boundaries issues in the transition from face-to-face talking therapy to online therapy in the time of Covid-19. Studia Universitatis Babes-Bolyai-Sociologia, 66(2), 113-123.
Mondal, I., Anand, N., Sharma, M. K., Kohli, T., Thakur, P. C., Kande, J. S., … & Ajith, S. J.
(2020). Telephonic psychotherapy in India: A reminder of challenges in times of COVID-19. Asian journal of psychiatry, 53, 102432.
Smith, D., & Fitzpatrick, M. (1995). Patient-therapist boundary issues: An integrative review of theory and research. Professional psychology: research and practice, 26(5), 499. Stoll, J., Müller, J. A., & Trachsel, M. (2020). Ethical issues in online psychotherapy: A narrative review. Frontiers in psychiatry, 10, 498439.
Wu, K. S., & Sonne, J. L. (2021). Therapist boundary crossings in the digital age: Psychologists’ practice frequencies and perceptions of ethicality. Professional Psychology: Research and Practice, 52(5), 419.
::TSI Activities from Around the Country::

Telemedicine Practice Guidelines Training Program
Prof. (Dr) Umashankar S.
Managing Director Med.Bot | Honorary Secretary, Telemedicine Society of India
The Telemedicine Society of India organized a Fundamental Course on Telemedicine Practice Guidelines in Madurai at Meenakshi Mission Hospital and Research Centre and Aravind Eye Hospitals on June 22nd and 23rd, 2024, respectively. The half-day training program began with a pre-test, followed by a session on “Enhancing healthcare through telemedicine—past, present, and future” by Dr. R. Kim, Chief Medical Officer and President of the Telemedicine Society of India. This was followed by a session on “Telemedicine Practice Guidelines” conducted by Dr. Umashankar S., Managing Director of Arogyayati Private Limited and Honorary Secretary of the Telemedicine Society of India. Dr. Chandrashekar, Head of NABH, led a session on “medical prescriptions”. The program concluded with an interactive question-and-answer session and a post-test.
A total of 92 participants attended the training program in hybrid mode from various locations, including Madurai, Theni, Tirunelveli, Pondicherry, Chennai, Coimbatore, and West Bengal. The attendees comprised doctors, managers, program coordinators, and health workers involved in telemedicine practice. At the end of the program, participants were issued completion certificates. The mean pre-test score was 6 out of 15 and the mean post-test score was 12 out of 15. Analysis of the pre-test and post-test revealed that there was an increase in the knowledge level of Telemedicine Practice Guidelines.







Webinar on “Urological Cancers – Close the Care Gap”
Dr. Ankur Mittal,
All India Institute of Medical Sciences Rishikesh – Urology
MBBS, MS, MCh (Urology)|Secretary, TSI-Uttarakhand State Chapter
Department of Urology, AIIMS Rishikesh in association with Telemedicine society of India UK Chapter has successfully organized a comprehensive Social Awareness Program titled “Urological Cancers – Close the Care Gap” on 13th July 2024 at Main Auditorium, AIIMS Rishikesh to raise awareness and educate the public about urological cancers. The event was graced by the Honorable Governor of Uttarakhand, Lt. Gen. Gurmit Singh (Retd.), and saw active participation from the medical community, cancer survivors, and the general public.
Objectives
The primary objectives of the program were:
Raising Awareness and Educational Outreach: Educate the public on the symptoms, diagnosis, and treatment options for urological cancers.
Promoting Early Detection: Encourage individuals to seek medical advice promptly when symptoms arise.
Support and Empowerment: Provide a platform for cancer survivors to share their experiences and inspire others.
Community Engagement: Foster collaboration between healthcare providers, NGOs, and the public to launch a sustained awareness campaign.
Activities
The event was meticulously planned and included the following key activities:
Inaugural Ceremony: The program was inaugurated by the chief guest, The Honorable Governor of Uttarakhand, Lt. Gen. Gurmit Singh, along with AIIMS Rishikesh’s Executive director, Professor Meenu Singh. The ceremony marked the official start of the campaign to “Close the Care Gap”. The Honorable Secretary of Telemedicine Society of India, Mr. Umashankar S. was felicitated by the Organizing Secretary of the program, Dr. Ankur Mittal.
Book Launch and Helpline Introduction: The Honorable Governor and dignitaries on dais unveiled a book on urological cancers, “Hope and Healing,” written in both Hindi and English to cater to a diverse audience. Additionally, a dedicated helpline number (8126542780) was launched to provide information and support to individuals affected by Urological Cancers
Expert Talks: Prominent medical professionals, including Dr. Amlesh Seth (Head of the Department of Urology, AIIMS New Delhi) delivered insightful talks on the prevalence of urological cancers in Uttarakhand, the importance of early detection, and the latest advancements in treatment, including robotic surgeries.
Survivor Testimonials: Cancer survivors shared their personal journeys of battling urological cancer. Their stories highlighted the significance of overcoming hesitation and seeking timely medical intervention.
Interactive Sessions: The program featured interactive sessions where attendees had the opportunity to ask questions to experts and receive detailed answers about urological cancers. This segment aimed to clear misconceptions and provide accurate information to the public.
Educational Material Distribution: Patient Information leaflets (both Hindi and English) about various urological cancers were distributed to attendees, providing crucial information on recognizing symptoms, understanding treatment option, and the importance of regular health check-ups.
Cultural Program: A NukkadNatak (street play) performed by Nursing students of AIIMS Rishikesh creatively depicted the impact of Prostate cancer, engaging the audience in a meaningful way.
New Innovative Technologies: Helpline number was launched via e-curtains and the public could download Patient Information Leaflets and the new book by scanning the QR codes displayed at the venue.
Outcomes
The “Urological Cancers – Close the Care Gap” program achieved significant outcomes:
Enhanced Awareness: The program successfully raised awareness about urological cancers, particularly in the high Himalayan regions of Uttarakhand where the incidence is notably higher due to environmental factors.
Increased Engagement: The launch of the helpline and the distribution of educational materials ensured that the public has continuous access to information and support.
Empowered Survivors: The testimonials from cancer survivors provided hope and motivation to current patients, emphasizing that early detection and treatment can lead to successful outcomes.
Collaborative Efforts: The event highlighted the importance of collective efforts involving healthcare professionals, NGOs, and the community to sustain an ongoing awareness campaign.
Positive Feedback: The interactive sessions received positive feedback from attendees, who appreciated the opportunity to engage directly with experts and clarify their doubts.
New Avenues: The program has opened up new options of collaborations between TSI, AIIMS Rishikesh and various NGOs for the benefit of patients.
In conclusion, the “Urological Cancers – Close the Care Gap” program, organized by the Department of Urology AIIMS Rishikesh in collaboration with Telemedicine Society of India UK Chapter, marked a significant step towards raising awareness, promoting early detection, and fostering a supportive community for individuals affected by urological cancers. The event’s success underscores the need for continued efforts to educate and empower the public in the fight against cancer.
Glimpses of the event



Webinar on “Seasonal Diseases – Rational Approach”
Dr. Raj Raval,
Founder & CEO Entel Healthtech | EC member-TSI Hqrs | President, TSI- Gujarat State Chapter
Date: 29th June 2024
Organizer: TSI- Gujarat State Chapter in association with ISCCM, IMA Gujarat
TSI Gujarat branch has organized webinar on ‘UPDATES ON SEASONAL DISEASES’ on 29th June 2024.
The meeting was well attended by all TSI members. It was also attended by members outside Gujarat.
Dr. Vivek Dave has delivered a talk on MONSOON DISEASES, Dr. Irsan Trivedi has discussed about SUMMER ILLNESSES, Dr. Raj Rawal has spoken about WINTER DISEASES. The webinar is well conducted by Dr. Chinmay Shah.
It was very interactive and informative session.
TSI Gujarat members have discussed about membership drive, various activities and future plans.
::ANNOUNCEMENTS::
To Register for the conference visit https://www.telemedicon2024.com/
Telemedicine – News from India & Abroad
AI-Powered Video Test Revolutionizes Parkinson’s Disease Diagnosis
A video-processing technique developed at the University of Florida, utilizing artificial intelligence……. Read More
Healthcare Providers Share Experiences Developing AI for Social Determinants
Social determinants of health refer to the circumstances in which individuals are born, grow, live, work, and age, encompassing
factors such as income………. Read More
Discover the Future of Vein Detection Technology
Anand Mahindra, Chairman of Mahindra Group, demonstrated a vein-detecting technology using infrared light in a video on X….. Read More
AI-Powered Nasal Endoscopy: Enhancing Precision and Outcomes
New study investigates how convolutional neural networks (CNNs) can enhance nasal endoscopy accuracy and efficiency…….. Read More
Telemedicine Practice Guidelines – A Foundation Course for RMPs by TSI Faculty
To know more about the Telemedicine Foundation Course click on the link below:
https://tsitn.org/tpg-course/
TSI invites all the TSI Chapters and Members to submit information on their upcoming Webinar or Events (50 words), News related to Telemedicine (200 words) or short articles (500 words) for the monthly e-newsletter.Guidelines for submission to TSI Newsletter-
- Report can be from 500 to 600 words
- Report Should be relevant to Telemedicine or Medical Informatics
- No promotion of self or any product
- Avoid plagiarism
- All references should be included
- Provide any attributions
- Visuals are welcome including video links
- Send full authors name, degrees, affiliations along with a passport sized photograph of good resolution. If multiple authors only main author photo to be sent.
Submission may be sent to – tsigrouptn@gmail.com
Editors reserve the rights for accepting and publishing any submitted material.
Editor in Chief – Dr. Sunil Shroff
Editors – Dr. Senthil Tamilarasan & Dr. Sheila John
Technical Partner- https://www.medindia.net






























































































 9. Himachal Pradesh Chapter on May 13, 2023: With active support and lead role by Dr. Vikrant Kanwar of AIIMS Bilaspur and wishes of Dr. Vir Singh Negi, Executive Director AIIMS, Bilaspur, the HP chapter was inaugurated on May 13, 2023. This is personally special and dear to me as this is my birthday celebrated in a satisfying way with the inauguration of a new chapter in an important hilly state of India. Dr. Vikrant also came to Telemedicon2022 at Goa and joined a parallel meeting with me along with Dr Arti Pawaria of Haryana and got motivated to form a state chapter and continued the work soon after going back. Another pleasant news is the state chapter soon after formation has come forward to host 2024 Telemedicon at HP in Dharamshala (Kangda) in Nov 2024 which was ratified by the 2023 AGM.
9. Himachal Pradesh Chapter on May 13, 2023: With active support and lead role by Dr. Vikrant Kanwar of AIIMS Bilaspur and wishes of Dr. Vir Singh Negi, Executive Director AIIMS, Bilaspur, the HP chapter was inaugurated on May 13, 2023. This is personally special and dear to me as this is my birthday celebrated in a satisfying way with the inauguration of a new chapter in an important hilly state of India. Dr. Vikrant also came to Telemedicon2022 at Goa and joined a parallel meeting with me along with Dr Arti Pawaria of Haryana and got motivated to form a state chapter and continued the work soon after going back. Another pleasant news is the state chapter soon after formation has come forward to host 2024 Telemedicon at HP in Dharamshala (Kangda) in Nov 2024 which was ratified by the 2023 AGM.

 11. Jharkhand Chapter on Aug 18, 2023: With active support and membership drive by Dr.Maishraj of AIIMS Deogarh, the Jharkhand chapter of TSI was inaugurated on Aug 18, 2023 under the aegis of President TSI Dr. Meenu Singh and Dr. Saurabh Varshney, Director AIIMS.
11. Jharkhand Chapter on Aug 18, 2023: With active support and membership drive by Dr.Maishraj of AIIMS Deogarh, the Jharkhand chapter of TSI was inaugurated on Aug 18, 2023 under the aegis of President TSI Dr. Meenu Singh and Dr. Saurabh Varshney, Director AIIMS.
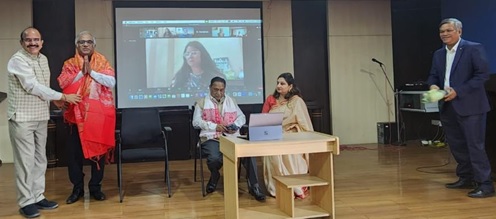
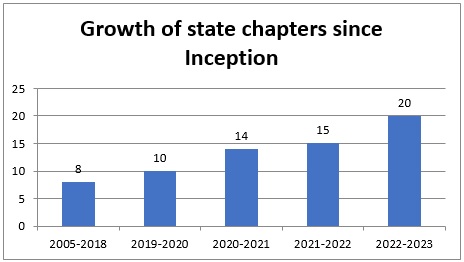
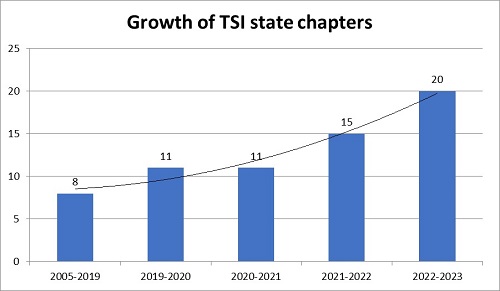 Though the growth of state chapters across the regions is increasing and pleasant to be noted, more and more activities are expected to be taken up under the aegis of these chapters with active participation by more members and particularly the younger generation. While conducting online/offline seminars and workshops or trainings is an initial and minimal activity to be taken up, the next and expected step in the journey is conducting some remote/rural camps with real usage and utilization of Telemedicine in practice.
Though the growth of state chapters across the regions is increasing and pleasant to be noted, more and more activities are expected to be taken up under the aegis of these chapters with active participation by more members and particularly the younger generation. While conducting online/offline seminars and workshops or trainings is an initial and minimal activity to be taken up, the next and expected step in the journey is conducting some remote/rural camps with real usage and utilization of Telemedicine in practice.



 Quiet unexpectedly but most pleasantly, the state chapter within a period of 9 months from the formation, came forward to successfully host the mid-term conference of 2022 on Aug 26, 2022 again at the prestigious SKIMS. The participation of several young doctors and particularly students and their presentation of high quality research papers was an added attraction in the mid-term conference.
Quiet unexpectedly but most pleasantly, the state chapter within a period of 9 months from the formation, came forward to successfully host the mid-term conference of 2022 on Aug 26, 2022 again at the prestigious SKIMS. The participation of several young doctors and particularly students and their presentation of high quality research papers was an added attraction in the mid-term conference.







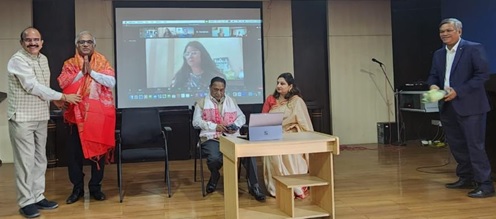








 Dr. Selvakumar: Thanks to dr ratta Speakers were off high quality Introduction of dr Ganapathy for quiz was amazing Time management personally by dr ratta was super Food quality was very tasty and rich started by exacises to reduce my calories Overall the the conference was of 7 star ratting Exhibit showcasing was in par excellent ENTERTAINMENT WAS SUPER WITH FUN THANKS to dr ratta again single man show lessons to be learnt from him how to manage such conferences My sincere thanks and appreciattin to old EC team with spl thsnks to dr murthy for excellent management for the last 4 yrs Welcome to the new EC team ism sure this team will tske to greater heights with leadership of dr kim Members absence was only defect in telelmedicon confrence atl we should have double the attendance Nothing more can be done by the TSI in showcasing yearly event I thsnk all the members who attended for the grouth of TSI the meet with there support.
Dr. Selvakumar: Thanks to dr ratta Speakers were off high quality Introduction of dr Ganapathy for quiz was amazing Time management personally by dr ratta was super Food quality was very tasty and rich started by exacises to reduce my calories Overall the the conference was of 7 star ratting Exhibit showcasing was in par excellent ENTERTAINMENT WAS SUPER WITH FUN THANKS to dr ratta again single man show lessons to be learnt from him how to manage such conferences My sincere thanks and appreciattin to old EC team with spl thsnks to dr murthy for excellent management for the last 4 yrs Welcome to the new EC team ism sure this team will tske to greater heights with leadership of dr kim Members absence was only defect in telelmedicon confrence atl we should have double the attendance Nothing more can be done by the TSI in showcasing yearly event I thsnk all the members who attended for the grouth of TSI the meet with there support. Dr. Raj Raval, Gujarat Chapter of TSI: On behalf of TSI GUJARAT CHAPTER, I’m thanking Dr.Ratta sir for involving us in organising squad although he knows he was very much able to do own his own. We learnt lot many things from him. He literally took all the pains to deliver wonderful event to us. Contents, New ideas pitching, timings, industries participation, food , cruise….everything were fabulous.
Dr. Raj Raval, Gujarat Chapter of TSI: On behalf of TSI GUJARAT CHAPTER, I’m thanking Dr.Ratta sir for involving us in organising squad although he knows he was very much able to do own his own. We learnt lot many things from him. He literally took all the pains to deliver wonderful event to us. Contents, New ideas pitching, timings, industries participation, food , cruise….everything were fabulous. Dr. Satyamurthy: You are incredible Dr.Selva. Nice to see your remarks. Dr.Ratta was the dream boy organiser of utmost sincerity, commitment and recorded his hattrick of conducting 3 TSI conferences with grand finale of taking you all on Cruise ship which I missed. God bless our group young Margadharshaks.
Dr. Satyamurthy: You are incredible Dr.Selva. Nice to see your remarks. Dr.Ratta was the dream boy organiser of utmost sincerity, commitment and recorded his hattrick of conducting 3 TSI conferences with grand finale of taking you all on Cruise ship which I missed. God bless our group young Margadharshaks.